What is Pediatric Myocarditis in Children?
Myocarditis is a condition where the muscular walls of the heart become inflamed. Myocarditis typically results in poor heart function.
There are many causes of myocarditis, including:
- Infection
- Medications
- Chemicals
- Radiation
- Certain diseases that cause inflammation in many different organs of the body
In most children, myocarditis is triggered by an infection, usually viral, involving the heart.
There are no known risk factors for developing myocarditis. Age, sex, and genetic make-up may all play a role in how severe the disease becomes once you have it.
Treatment for myocarditis is based on how badly the heart is affected. Many children have a complete recovery, but some may develop serious heart failure and require chronic care from a cardiologist.
Causes of Myocarditis
In children, viral infections are the most common causes for myocarditis. The most common viruses involved are:
- Parvovirus
- Influenza virus
- Adenovirus and coxsackie virus
- Viruses such as rubella, rubeola and HIV
Rarely, bacteria such as those causing Lyme disease, Rocky Mountain spotted fever, or toxic shock syndrome, or fungus or parasites can cause myocarditis. It is important to recognize that even though a child may have one of these infections, it is rare to develop myocarditis.
When myocarditis is caused by an infection, the germ first infects the heart. The germ enters the body and travels through the bloodstream to the heart. It grows and reproduces within the heart. It may cause some cell damage as it spreads from one cell to another.
Normally, the immune system will go to the site of the infection to get rid of the germ. In some children, this response is over-aggressive so that not only the germ is destroyed, but the heart cells themselves may be damaged.
Most of the damage to the heart is caused by the body’s immune reaction to the germ, and not by the germ itself. It is unclear why this happens in some children. The abnormal immune response may be confined to a small area or involve a large portion of muscle tissue. Often, the more heart muscle that is damaged, the more severe the symptoms. There are other triggers for myocarditis. Many drugs used for chemotherapy and certain antibiotics in rare cases can cause an immune response similar to what is seen with viral infections.
Children with diseases such as lupus, rheumatoid arthritis, ulcerative colitis, and scleroderma (diseases that involve inflammation of many different organs of the body) may also develop myocarditis, but this is rare. The reason for getting an abnormal immune response under these conditions is not as well understood.
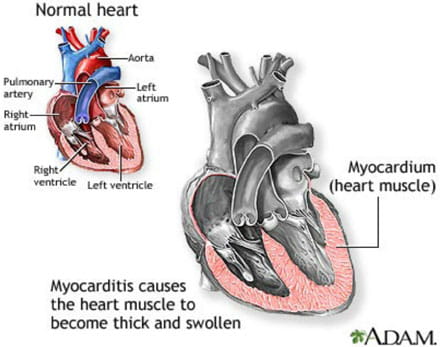
Myocarditis and the Heart
The inflammatory process begins when the body's immune cells (the cells that fight infection) actually penetrate the heart tissue. These immune cells become activated and produce chemicals that can cause damage to the heart muscle cells. There is thickening and swelling of the heart muscle. All four chambers of the heart may be affected and become enlarged.
Damaged muscle cells may heal over time or there may be cell death followed by scar formation. If this process is extensive and a large portion of the heart is involved, the heart's ability to pump blood is impaired.
As a result, the key organs and tissues in the body do not get enough oxygen and nutrients and cannot get rid of waste products. This is often referred to as congestive heart failure.
It is not unusual for someone who has severe myocarditis to suffer from other problems such as liver or kidney failure, as well.
Signs and Symptoms of Myocarditis
The symptoms of myocarditis may be subtle, making the diagnosis difficult, or the child may have obvious symptoms of heart failure. Clinical experience has shown the severity of symptoms or illness usually depends on the age of the child.
Children over 2 years of age may have fewer symptoms than newborns and infants who are usually more severely affected. This is thought to be due to the immaturity of a baby's immune system.
A child may get an infection during pregnancy (Rubella, for example) when it travels from the mother to baby. They are often breathing fast and having trouble feeding. They can be very fussy and difficult to console or very tired and sleep more than normal.
Blood will not travel through the body as well, and infants may have cool, pale hands and feet. The kidneys may also not work properly and there will be less urine produced.
There may be fever or other evidence of infection. In older infants, the findings are similar but there may be an associated weight loss due to trouble feeding.
Older children may have fewer symptoms. They may complain of a flu-like illness with of fatigue, malaise and fever.
They may not be able to tolerate exercise or may complain of chest pain or palpitations (skipped or extra heartbeats). They may develop a cough. Some children who have congestive heart failure may also have swelling in the face, feet or the legs. There may be belly pain and nausea due to swelling of the liver.
Due to poor blood flow, the liver and kidneys may be injured. The signs and symptoms of myocarditis are subtle early in the illness; therefore, it is not unusual for myocarditis to go unrecognized.
Myocarditis is sometimes diagnosed in retrospect when the child has an abnormal heart rhythm or is critically ill. It can also be diagnosed retrospectively in adulthood with abnormal heart rhythm or an enlarged heart.
Diagnosis of Myocarditis
Unfortunately, to the frustration of parents and doctors, there is no specific test for myocarditis. It is mostly a clinical diagnosis where the doctor must rely on the history provided by the family and physical examination of the child.
There are many tests that can be performed that help with making a diagnosis of myocarditis.
- The most common test is a chest X-ray. Often the heart size is enlarged, the blood vessels of the lungs are bigger, and fluid may enter the lungs.
- An electrocardiogram can also give helpful clues if the diagnosis is suspected; however, the findings may be non-specific. There may also be abnormal heart beats that can occur with myocarditis.
- An echocardiogram or heart ultrasound can be used to look at heart size and overall function. This helps confirm the clinical diagnosis as well as rules out the presence of blood clots inside the heart. Blood clots can form when the blood does not move easily through the heart.
- Other blood tests may help to see how well the liver and kidneys are working. A blood count and specific tests for infections may also be done.
- The most precise way to make the diagnosis of myocarditis is by doing a heart biopsy during a cardiac catheterization. This involves the use of a long catheter that is passed up a large blood vessel in the leg. Once the catheter is in the heart, a tiny piece of heart muscle is taken and sent to the pathologist to look at under the microscope.
Results vary but the diagnosis of myocarditis is made by this method up to 65 percent of the time. The results of the biopsy are not 100 percent because the areas of the heart affected by the inflammation are often patchy and may be missed.
Treatment of Myocarditis
The inflammation in the heart muscle will usually go away on its own. There is no cure for myocarditis. In general, the goal of medical therapy is to support the heart function so that adequate blood circulation is maintained. Most children diagnosed with myocarditis are admitted to an intensive care unit for initial management and careful monitoring.
Medicines to help the heart work better, either by controlling the blood pressure or by improving the ability of the heart to pump blood, are the first line of treatment. One or more of these medicines may be used, depending upon the severity of the myocarditis. A diuretic can also help clear extra fluid from the lungs or other body tissues.
There are also medicines currently under investigation that help decrease the abnormal immune response.
One drug frequently used is called intravenous immunoglobulin (IVIG), which consists of purified antibodies, the substances that the body's immune cells produce to fight infection. Although it is not understood exactly how this works, it has been shown to slow down the inflammatory process. Patients treated with IVIG appear to have fewer long-term heart complications.
Medicines to prevent the formation of blood clots in the heart may be given. These medicines are used since a clot may form when the heart does not pump efficiently.
Medicines to eliminate the virus are not typically used because this rarely alters the course as most of the damage from the infection occurs early. Antibiotics are not helpful because viruses cause most myocarditis. Treating autoimmune disorders, typically with steroids, is helpful when this is the cause of the muscle inflammation.
Most children diagnosed with myocarditis are admitted to an intensive care unit for initial management. It is important for the child to be placed on bed rest. There is evidence to suggest that strenuous activity may be harmful to the heart during the recovery period. Depending upon the severity of the myocarditis, this may mean that physical activity is restricted for weeks to months. The child’s physical activity should be slowly increased over time.
Long-Term Outlook
The good news is that about two-thirds of the children, with the right medical management, will have a complete recovery.
If untreated, only 10 percent to 20 percent will have recovery on their own, and 80 percent will develop chronic heart disease. For most children, recovery usually occurs within two to three months from the onset of the illness.
Of the remaining one-third who are treated, 10 percent to 20 percent will improve but have chronic residual heart problems called “dilated cardiomyopathy.”
This is a condition where the heart has become enlarged and may have diminished function or residual heart failure. In this case, the child will need long-term follow-up by a cardiologist. Sometimes these children will develop progressive heart failure and need a heart transplant.
Other children may be at risk for having heart rhythm problems. These can often be treated with medicine.
The population that is at the highest risk for serious disease is newborns. The mortality rate is as high as 50 percent to 70 percent. When this is the case, there is a high risk of sudden death and some children may need a heart transplant urgently. This severity of disease is rare and therefore represents a very small number of children.



