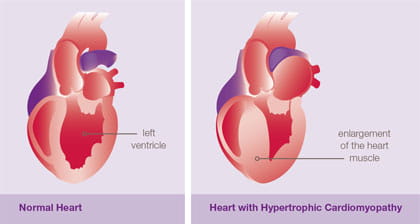
What is Hypertrophic Cardiomyopathy (HCM)?
Hypertrophic cardiomyopathy (HCM) is a condition of heart muscle disease in which the muscle is thickened (hypertrophic). This thickening typically occurs in the lower left chamber of the heart, called the left ventricle. Thickening of the heart muscle can occur at the septum (muscular wall that separates the left and right side of the heart), the posterior wall or free wall (outside wall of the left ventricle), the apex (the bottom of the heart) or throughout the entire left ventricle. When the muscle becomes thickened, it may make it difficult for an efficient amount of blood to flow into and out of the heart, especially during exercise. In some cases, the thickening of the muscle can block blood flow from the left ventricle to the aorta. This is called “outflow tract obstruction.
The cardiomyocytes (heart muscle cells) in individuals with HCM have characteristic features. Under a microscope, the cells appear disorganized and irregular (myocyte disarray). This disarray may cause changes in the electrical signals traveling through the lower chambers of the heart and lead to ventricular arrhythmias (abnormal heart rhythm). Hypertrophic cardiomyopathy affects an estimated 600,000 to 1.5 million Americans, or one in 500 people.