Partnership of Donors Fuels Better Research, Better Care
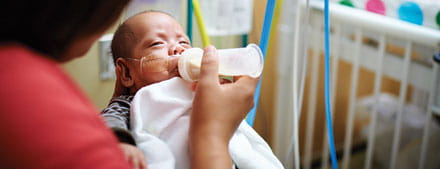
In the NICU, Jeremy, born prematurely, has progressed to bottle feeds.
Andrew South, MD, MPH, wears two hats, professionally speaking.
As a physician in the newborn intensive care unit (NICU) at Cincinnati Children’s, he provides medical care and treatment to the sickest, most fragile babies in Greater Cincinnati. As a researcher, he works to learn more about necrotizing enterocolitis (NEC) − one of the most common and deadly ailments affecting the premature babies he cares for every day.
Occurring in approximately 10 percent of very low birth weight infants, NEC has a 40 percent fatality rate − and infants who survive can have ongoing complications, including intestinal disorders and developmental delays. What’s more, because it predominantly affects premature and medically fragile infants, it is a difficult disease to study and, as a result, very little is known about NEC.
Even diagnosing the disease and predicting its severity are difficult.
That’s why, when Cincinnati Children’s developed the world’s first infant-sized magnetic resonance imaging (MRI) machine, South immediately saw its potential for research on NEC. Located within the NICU, this revolutionary MRI is designed and sized specifically to safely image the most fragile infants while keeping them close to the critical equipment and care professionals they need. No longer do sick babies need to be transported from the NICU to an MRI elsewhere in the medical center.
For both clinical and research applications, this unique MRI is nothing short of transformational.
“The NICU MRI gives us a tool we’ve never had before − one that can help us lay a baseline for normal development and help us spot abnormal development more quickly. The potential for discovery with the MRI is astounding,” says South.
Thanks to the generosity of an anonymous donor, South was able to initiate the world’s first MRI research project on NEC not long after the infant-sized MRI was up and running. In fact, the research this technology enables is so new, researchers using it often are not eligible for funding from traditional sources, such as the National Institutes of Health.
“Traditional funders typically want to support research that’s seen some success already. Yet funding is vital to get new approaches − like our NEC studies − off the ground. We were fortunate to have a family willing to step in and help us fund this study from the beginning,” South explains.
Even more remarkable, this family’s generosity isn’t borne of a personal experience as a patient family in the NICU. It was sparked by a family members’ experience volunteering to care for fragile babies.
“Using the MRI to study these babies and NEC could lead to a profound transformation of our understanding of gastrointestinal development.”
South pauses. “It will help us diagnose NEC earlier, start treatment sooner, save more lives, and get babies home safely with their families − where they belong.”
For the family whose gift supports South’s work, that’s the most important reason of all. They understand that groundbreaking care starts with cutting-edge research. And, thanks to their help, South and his team may one day see a newborn ICU with fewer cases of NEC and babies who leave for home sooner than ever before.




