Daily Operations
The link between capacity management and safe care has been key to our success. It was not until we recognized this link that our efforts began to have an impact. It allowed us to shift our focus from bed availability to whether kids were receiving care from the right teams. We began active and systematic measurement of our failures to identify where and why those failures were taking place. We recognized that through measurement, we would have a way of knowing whether our changes were resulting in improvement. We implemented a daily bed huddle to allow us to plan needs across our complex and interdependent system. The huddle connected the work we were doing on flow to patient safety and family experience, thus integrating three key strategic goals.
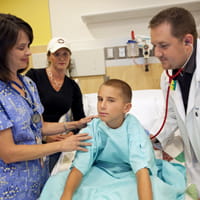 Fundamental to all of our flow work is demand / capacity matching. Whether we’re planning tomorrow’s transfer of a patient from the PICU to the neuroscience unit, or the next new inpatient space, our focus is on reliably matching capacity to demand. Our uses of operations management tools and improvement science are helping us understand and manage artificial variation (anything that is influenced primarily by people and their behaviors / schedules) and predict natural variation (such as an increase in volume due to flu season or a patient’s response to a therapy). We began our work in daily operations on our inpatient and perioperative areas and are now expanding it into areas such as outpatient clinics and the Emergency Department.
Fundamental to all of our flow work is demand / capacity matching. Whether we’re planning tomorrow’s transfer of a patient from the PICU to the neuroscience unit, or the next new inpatient space, our focus is on reliably matching capacity to demand. Our uses of operations management tools and improvement science are helping us understand and manage artificial variation (anything that is influenced primarily by people and their behaviors / schedules) and predict natural variation (such as an increase in volume due to flu season or a patient’s response to a therapy). We began our work in daily operations on our inpatient and perioperative areas and are now expanding it into areas such as outpatient clinics and the Emergency Department.
Regardless of location, demand / capacity matching revolves around the following key concepts:
Managing Artificial Variation
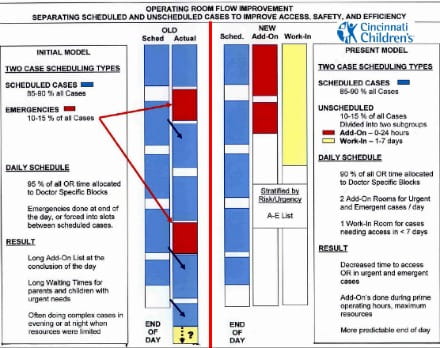
Managing artificial variation is inherently demand focused. Our efforts include smoothing (i.e., decreasing daily schedule variation) and predicting bed need. To accomplish this, we started with the largest population of scheduled admissions – the surgical schedule – and one of our most limited resources – pediatric ICU (PICU) beds. We require that surgeons predict their inpatient bed needs and incorporate that information into the flow plan for a patient. By designating PICU beds as a resource in the surgical schedule, we are able to limit PICU admissions and control the artificial variation in PICU admissions.
Managing Discharges to Create Capacity
Managing discharges effectively and safely revolves around having clinical care teams effectively develop and execute plans of care that enable patients to be discharged without delay and after completion of appropriate care. We achieved this by testing and developing several tools, many of which are linked to our electronic medical record system. These include discharge prediction models, a discharge checklist and evidence- based guidelines for plan of care.
| >See a document (.pdf) that measures the percentage of patients who are discharged during or before their predicted four-hour discharge window. Predictions are collected at 7 am and again two hours before every shift change. |
Managing Internal Patient Transfers
Managing internal patient transfers focuses on efficiently moving patients through our system without delay. We use many of the basic tools developed for discharge planning, but which have been adapted for internal transfers. For internal patient transfers from ICUs and post-operative recovery units, prediction is especially important to allow identification and the setting aside of specific beds. Unscheduled transfers, such as inpatient admissions from the ED, require the prediction of natural variation. We have done this by creating a tool based on historical volumes and the percent of ED visits typically admitted. A percentage of that prediction is added to allow for admissions from the community.





