What is Appendicitis?
The Appendix
Your appendix is a small, tube-shaped piece of tissue. It is found in the lower right part of the belly. It is attached to the large intestine. A healthy appendix makes mucus. This mucus drains into the large intestine. Appendicitis refers to an inflamed or infected appendix. It happens when the appendix becomes blocked. Many things can cause a blockage in the appendix. Some of them include dried mucus, hard stool, and parasites such as pinworm.
When the appendix becomes blocked, the mucus the appendix makes builds up and hardens. The backed-up mucus stops normal blood flow through the appendix. This causes the appendix to become inflamed and swell. Over time, the infection and swelling can cause the appendix to perforate (burst or rupture). If not treated, infection can spread all through the belly (called peritonitis).
An inflamed or infected appendix is called appendicitis. Appendicitis is the most common reason for emergency belly surgery in kids. It is a little more common in boys. Most cases of appendicitis happen in kids between 8 to 16 years old. Kids younger than 5 have a much higher chance of having a burst appendix. This is because it is harder for them to describe their pain. It is harder for them to tell exactly where it hurts. It is also harder for them to sit still while a doctor checks them out.
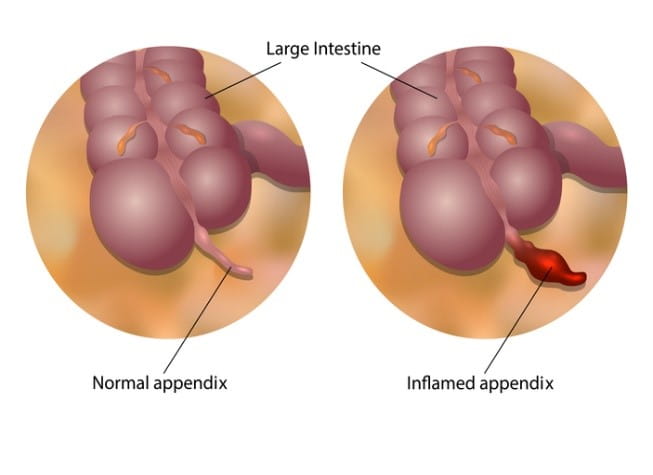
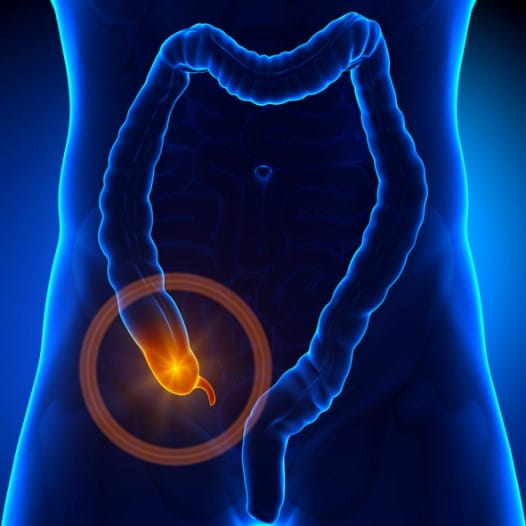
Signs of An Infected Appendix
Not all kids have all signs. The most common signs are:
- Pain in the middle of the belly. The pain starts at the belly button and moves down to the right lower part of the belly. This is where the appendix is found. The pain usually gets worse over time.
- Pain with moving. Pain with deep breaths. Pain with coughing or sneezing.
- Pain when someone pushes on the belly.
- Not hungry.
- Feeling sick to the stomach.
- Vomiting.
- Fever and / or chills.
- Diarrhea.
- Pain with peeing.
Diagnosis of Appendicitis
The doctor will talk to you about any other health problems your child has had. The doctor will also do a full exam on your child. This helps the doctor make the right diagnosis. Tests that may be done to diagnose appendicitis include:
- Belly (abdominal) ultrasound – Warm gel is put on the belly, and a wand uses sound waves to take pictures of the appendix. If the appendix has burst, the appendix may not be seen. If the appendix is behind the intestine, it may not be seen.
- CT scan – this may be done if the appendix can’t be seen with an ultrasound. The CT scan uses x-rays to take pictures of the organs inside of the belly.
- Blood tests –this can show if there is an infection.
- Urinalysis – this can show if there is an infection of the bladder (urinary tract infection) or the kidneys. This can sometimes look like appendicitis.
Treatment of Appendicitis
Antibiotics: If the appendix has not burst, treatment with only antibiotics may be possible. Your doctor will talk to you if this is an option.
Appendectomy:
- Most kids with appendicitis will need surgery to remove the infected appendix.
- Treatment is different for a burst appendix compared to one that has not burst.
- All patients will get IV antibiotics before surgery.
- Only patients with a burst appendix will get IV antibiotics after surgery.
- Surgery will be done in one of three ways:
- One incision through the belly button – this is more common if the appendix has not burst.
- Three port surgery – three small incisions are made in the belly.
- Open appendectomy – this is very rare. It is usually done in cases where the appendix burst a few days before the surgery and the inside of the belly is very infected (called peritonitis).
- Sometimes, when the appendix was burst for a long period of time, the appendectomy is done later. When this happens, your child will get IV antibiotics for a few days. You will then go home and come back to the hospital in six to eight weeks to have the appendix removed. This is known as an interval appendectomy.
- Learn more about our surgery program.
Hospital Stay
If the appendix did not rupture, most patients go home between two and 24 hours after surgery. Once they can drink clear liquids and have peed, your child may be able to go home.
If the appendix was ruptured, the hospital stay is usually between three to seven days.
If the appendix was ruptured, your child may have a tube going from their nose to their belly (called an NG tube). This tube helps keep the stomach empty. It takes a while for the belly to wake up from the infection and the surgery. Until the belly wakes up, your child may feel sick to their stomach (nausea). They may not want to eat. Once your child’s belly wakes up, they don’t feel sick to their stomach, and they can drink, the tube in their nose can come out. Your child may have diarrhea for a few days after surgery.
If the appendix was ruptured, your child will get IV antibiotics until their white blood cell count comes down or until they go home. If their white blood cell count is still a little high, they may be prescribed an antibiotic to take by mouth after they go home.
For a ruptured appendix, your child may be able to go home when the following goals are met:
- Their belly wakes up.
- They no longer feel sick to their stomach.
- They can eat.
- They do not have a fever.
Guidelines for post-discharge care after appendectomy
Day One and Day Two
Wound Care
- Keep incisions dry
- Do not remove clear plastic dressing over incision until day two
Bathing
- Do not take a bath
- Do not take a shower
Activity
- Walk at least every hour
- Can to go to school if you feel up to it
- No gym or contact sports
- Do not lift more than 20 pounds – including backpack
Pain Medicine
- Acetaminophen every six hours
- Ibuprofen every six hours
- Alternate Ibuprofen and Acetaminophen every three to four hours; do not take them at the same time
Day Three
Wound Care
- Do not remove SteriStrips or Dermabond (glue)
Bathing
- Do not take a bath
- Okay to take a shower
- Wash incisions gently with soap
- Rinse with water
- Pat dry, do not rub
Activity
- Can go to school
- Do not lift more than 20 pounds – including backpack
- No gym or contact sports
- No swimming
Pain Medicine
- Acetaminophen or Ibuprofen if needed
- Do not take at the same time
Day Seven - One week after surgery
Wound Care
- Do not remove SteriStrips or Dermabond. They will fall off on their own.
Bathing
- Okay to take a bath now
Activity
- Almost all patients should be back at school by this time
- Do not lift more than 20 pounds – including backpack
- No gym or contact sports
- Okay to swim in clean, chlorinated water
- Not okay to swim in lakes, rivers, oceans
Pain Medicine
- Most patients do not need pain medicine by this point
Day 14 - two weeks after surgery
Wound Care
- SteriStrips or Dermabond should have fallen off or flaked off – if not, it is okay to gently remove them by loosening them up with a clean, warm, damp washcloth before gently peeling them off.
Bathing
- No restrictions
Activity
- Okay to lift more than 20 pounds
- Okay to carry backpack
- Okay for gym and contact sports
- Okay to swim in lakes, rivers, oceans
Pain Management
Before surgery: Acetaminophen (Tylenol) is used to manage pain before surgery. If the pain is severe, an opioid medication such as Morphine may be used.
During surgery: An anesthesiologist (anesthesia doctor) will manage your child’s pain during surgery. Different pain medications will be used. All patients will get a pain medicine injected around the incisions at the end of surgery. This will help decrease pain after surgery.
Pain management after surgery: Most patients will have some pain for the first few days after surgery. The goal is to keep the pain at a level where your child can move, talk, and take deep breaths. Your child needs to do all these things soon after surgery. The more they move, the better they will feel, the less pain they will have, and the sooner they will be able to go home.
If the appendix did not rupture, Acetaminophen (Tylenol) and Ibuprofen (Motrin or Advil) are enough to manage pain. It is rare to need stronger pain medicine.
If the appendix ruptured, Acetaminophen (Tylenol) and Ibuprofen (Motrin or Advil) or Toradol will be given around the clock for the first two days after surgery. Opioid medications are usually not needed. They are only given when your child’s pain is severe and does not get better with the other pain medications.
Patients almost never go home with opioid medications at discharge. Learn more about how to treat pain after surgery.
Pain management after you go home:
You should alternate Acetaminophen (Tylenol) or Ibuprofen (Motrin or Advil) every three hours for the first two days after you go home. It depends on what your child needs.
You should not take Acetaminophen and Ibuprofen at the same time. The correct dose for both Acetaminophen and Ibuprofen will be included with your discharge instructions. Acetaminophen and Ibuprofen dosages are based on your child’s weight. A prescription for both can be sent to the pharmacy of your choice. However, insurance does not usually pay for it.
For your convenience, Cincinnati Children’s Outpatient Pharmacy has low-cost Acetaminophen and Ibuprofen at both the Main campus and the Liberty locations.
Burnet Campus: Located on the ground floor between the Welcome Desk and Gift Shop
Liberty Campus: Located near 2nd Floor Entrance near the Gift Shop
Find your nearest Cincinnati Children's Outpatient Pharmacy location.
Anxiety and Pain: Anxiety can happen when you have stress from not knowing what to expect. This is very common when your child is sick. It is even more common when surgery is needed. Watch the video below which explains how anxiety and pain go together:
Distraction Techniques to Help Limit Pain:
Some things that may help your child be more comfortable:
- Find a relaxing position. Try using blankets or pillows to help create a comfortable space. Hold or rock your child as allowed by your child’s care team.
- Distract with activities. Help keep your child’s mind off the pain with music or quiet activities. Suggestions for activities are watching a video or using hand-held electronics.
- Distract with talking. Talk about things not related to the hospital or surgery. Things to talk about with your child may include friends, favorite movies, favorite toys or games, their pets, or school.
- Use humor. It can improve your child’s mood and change their attitude.
- Talk about ways to cope. “If you do this _____, you will get better.”
- Encourage relaxation techniques. Try deep and steady breathing or meditation. Encourage relaxation techniques such as deep and steady breathing or meditation.
- Use cool or low heat. Ask your child’s care team if a cool or low heat source is okay to use. Make use of cool or low heat for comfort if it is okay.
Belly Pain and Constipation after Surgery: When your appendix is infected, the infection and inflammation slow down the movement of your child’s gastrointestinal (GI) tract. Surgery and anesthesia also cause your child’s GI tract to slow down. Before and after surgery, this can cause your child to feel sick to their stomach (nausea) and not want to eat. After surgery, it can cause constipation, making it harder for your child to poop. Miralax is an over-the-counter medication that can be used after surgery to help your child’s bowels move. Having your child drink plenty of water and walk often can also help decrease constipation.
Problems After an Appendectomy
An infection of the incision (cut on the skin) happens in about three of 10 kids after surgery. Signs may include:
- Incision becomes very red, “angry” looking.
- Incision may feel warm and / or tender to the touch.
- Incision may have green or yellow drainage.
- Drainage may smell bad.
- Fever and / or chills; and
- Feeling very tired.
- Your child may need to come see the surgery team in the office.
- Treatment may include antibiotics and / or drainage of the wound.
- An abscess, a local infection inside of belly that has not spread (i.e., a pus pocket), is more common when the appendix ruptured (burst) before surgery. Signs may include:
- Belly pain that does not get better with Ibuprofen or Acetaminophen.
- Belly pain that gets worse instead of better.
- Fever and / or chills.
- Feeling sick to the stomach or vomiting; and
- Diarrhea or pain when peeing
- You need to come back to the hospital if there is concern for an abscess.
- An Ultrasound or CT scan (cat scan) may be needed to diagnose an abscess.
- A radiologist may use ultrasound to find the abscess. Once the abscess is found, the radiologist may need to drain the infection to the outside of the body. Sometimes a drain will be left in the belly to the outside of the body for a few days. IV antibiotics are given and may be the only treatment needed if the abscess is small.
When To Call Us
You should call the surgeon’s office if any of the following things happen:
1.Your child has a fever over 101 degrees.
2.You child has an incision that is red, swollen, warm and / or very tender to the touch.
3.Your child has an incision that has pus or yellow/green tinged drainage. A small amount of clear yellow or blood-tinged drainage is common.
4.Your child has pain that is getting worse, especially if it does not get better after taking Acetaminophen (Tylenol) or Ibuprofen (Motrin, Advil); or
5.Your child has diarrhea that does not get better within two days of going home.
How to reach your child’s care team for questions or problems after surgery:
513-636-4371 – Call this number Monday through Friday from 8 a.m. to 4:30 p.m.
513-636-42009 – Call this number after 4:30 p.m. Monday through Friday, on weekends, and on holidays. This is the main hospital number. Please ask the operator to contact the surgeon on-call.
Please call 9-1-1 if your child is having a medical emergency such as trouble breathing or your child cannot be woken up.




