Hypospadias is a common structural difference of the penis where the urethra (the tube that carries pee from the bladder to outside of the body) is on the underside rather than the tip of the penis. The opening can be located anywhere from the glans of the penis to the skin between the scrotum and anus.
A condition called chordee is often seen with hypospadias. Chordee is a downward curve of the penis. This can occur with or without a hypospadias.
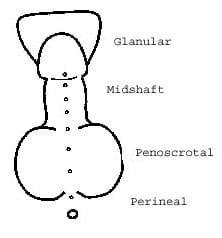
The types of hypospadias include:
- Distal or glandular: The most common form when the opening is found near the head of the penis
- Midshaft: Occurs when opening is found in the middle to the lower shaft of the penis
- Penoscrotal: This occurs when the opening is found where the penis and scrotum join
- Perineal: Occurs when the opening is behind the scrotal sac. These are the most severe forms of hypospadias, and are less common.
How Common Is This Condition?
Hypospadias occurs in one out of every 150-300 boys. If a boy has hypospadias, there is a 15% chance that his brother will have the condition. About 8% of fathers who have a son with hypospadias also have the condition.
What Causes This Condition?
The exact cause of hypospadias is unknown. There are many factors believed to be involved in its development. Genetics, the environment and hormones may be factors that influence the development of hypospadias.
How Is Hypospadias Diagnosed?
Usually, hypospadias is noticed at birth. Along with the misplaced opening, the foreskin is often incomplete and forms a hood. This is called a dorsal hood.
What are the Signs and Symptoms of Hypospadias?
Some boys with mild forms of hypospadias may have no symptoms from their hypospadias.
If the hypospadias and/or chordee is more severe and not repaired, children may have these issues as they grow:
- Urine stream may be hard to direct and control
- The penis may curve as he grows, causing sexual dysfunction later in life
- If the urethral opening is near or behind the scrotum, he may have fertility problems later in life
How is Hypospadias Treated?
Some patients with hypospadias do not have any treatment besides observation, due to no symptoms or patient/family preference. Surgical treatment of hypospadias and chordee can change the look of the penis and some patient/families choose this after discussion with their doctor.
No medicine will correct a chordee or hypospadias, and children are not expected to outgrow these anatomical conditions.
Surgery can often correct hypospadias. The care team may recommend surgery to:
- Bring the urethral opening to the tip of the penis. This allows a controlled stream of urine while standing.
- Straighten the penis (if chordee is present) to minimize the risk of painful intercourse later in life.
A pediatric urologist may need to use the foreskin as part of the surgical repair, so it is recommended that children with hypospadias not be circumcised at birth. Surgical repair usually takes place after four to six months of age, however it can be done later. The surgery is usually done on an outpatient basis while the patient is asleep, under general anesthesia. In the more severe forms of hypospadias, the surgical repair may be done in multiple stages.
Possible Complications
Hypospadias surgery may be very successful, but there can be some potential complications. In some cases, a hole or a fistula may occur, and urine may leak through the hole. More surgery may be needed to repair this problem. Scarring within the urethra may occur and cause the urethra to narrow. This may interfere with the passage of urine and would also need to be corrected with surgery.
Patients may need to return for checkups until after puberty.