What Are the Types of Dialysis?
Dialysis is a way to remove waste products and extra water from the blood of patients with kidney failure. The two main types of dialysis are hemodialysis and peritoneal dialysis.
Hemodialysis (HD)
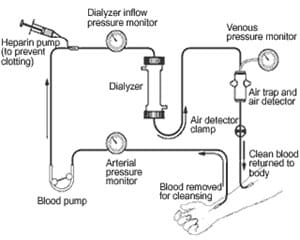
The Procedure
In hemodialysis, your blood is removed from your body, a few ounces at a time through some form of IV access. A machine pumps the blood through tubing to a filter, or dialyzer. The dialyzer is a canister that contains thousands of fibers that filter out the wastes and extra fluid. The clean blood is then pumped through tubing and returned to the body. Removing the harmful wastes and extra salt and fluids helps control blood pressure and keep the proper balance of chemicals like potassium and sodium in the body.
Adjusting to Hemodialysis
One of the biggest adjustments when starting hemodialysis treatments is following a rigid schedule. Hemodialysis is usually performed in a clinic under the supervision of a nurse and kidney specialist, and generally requires anywhere from three treatments a week (most common schedule) to five treatments a week. For example, a Monday-Wednesday-Friday schedule or a Tuesday-Thursday-Saturday schedule is possible. More frequent treatments might be needed for additional fluid removal and / or waste removal. Each treatment can take about three to four hours to complete. Options for scheduling treatments (including both the frequency and length of treatments) will be discussed before starting dialysis.
To perform hemodialysis, vascular access must be placed so the blood can be readily removed for the procedure. Vascular access is typically placed by a surgeon. Options for vascular access include creating a fistula (a surgery that directly connects an artery and vein, often in the arm), placing a graft (tubing under the skin that connects an artery to a vein; also often in the arm but can be placed in other parts of the body), or placing a dialysis catheter (a large IV catheter with two separate openings placed into a large vein). Fistulas and grafts involve placing IV needles through the skin to connect to the dialysis machine tubing and filter. Fistulas and grafts often need to heal for some amount of time prior to their use. And fistulas need to mature so that the blood vessel becomes large enough to stick with the needles. However, the benefit of fistulas and grafts is that they have a lower risk of infection, and they allow the patient to shower and swim. Patients with catheters have a higher risk of infections. They are not allowed to shower or swim due to these infection risks.
Peritoneal Dialysis (PD)
How Does Peritoneal Dialysis Work?
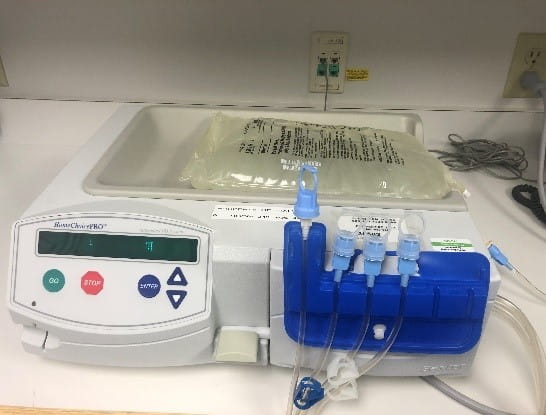
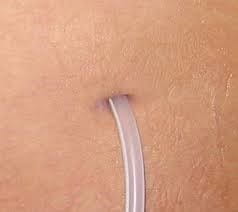
Similar to vascular access for hemodialysis, the PD catheter is also surgically placed. Ideally, the PD catheter insertion site is fully healed before the start of peritoneal dialysis. Once the catheter is fully healed, patients can shower regularly, take baths (as long as the exit site and catheter are not submerged), and swim in a private chlorinated or saline pool or the ocean. Because of the risk of infection, swimming in public pools, ponds, lakes and rivers is not allowed.
Two Types of Peritoneal Dialysis
Different types of PD will have different schedules of daily exchanges. One form of PD, Continuous Ambulatory Peritoneal Dialysis (CAPD), doesn’t require a machine but exchanges may be done manually a few times during the day. As the word ambulatory suggests, the patient can walk around with the dialysate solution in the abdomen. Another form of PD, Continuous Cycler-Assisted Peritoneal Dialysis (CCPD), requires a machine called a cycler to fill and drain the abdomen, usually at night while the patient is asleep. CCPD is also sometimes called Automated Peritoneal Dialysis (APD). The type of PD that is chosen for your child is based on a variety of factors, including medical, social and / or mental health-related circumstances.



