Regional Care Model Optimizes Care and Outcomes for Premature Infants
Clinical History and Presentation
In September 2009, a pregnant woman at 27 weeks gestation presented to a Cincinnati area hospital with elevated blood pressure. Her medical history was significant for chronic hypertension and her obstetric history was of one prior miscarriage. She was diagnosed with preeclampsia and started on magnesium sulfate.
Although the regional hospital had a Level II nursery, the woman’s physicians decided to transfer her to a hospital with a Level III nursery. Their decision was the result of a robust education campaign with area obstetricians regarding improved outcomes when infants younger than 32 weeks gestation are delivered at a Level III center. This is in keeping with current recommendations by The American Academy of Pediatrics and American Congress of Obstetricians and Gynecologists.
Our Approach
The neonatal intensive care unit (NICU) at the delivery hospital to which the patient was transferred is staffed by neonatologists from the Perinatal Institute at Cincinnati Children’s Hospital Medical Center. The patient was placed on bed rest on arrival and given two doses of betamethasone, which evidence shows reduces neonatal morbidities. Over the next five days, the baby had reversal of end diastolic flow on Doppler ultrasound — a sign of placental insufficiency — and the mother’s hypertension worsened. The NICU team prepared the family for the arrival of a preterm infant. Because the team believed both mother and infant would not tolerate labor, they proceeded with a Cesarean section delivery.
The baby girl was born at 28 weeks gestation and weighed 700 grams (1 lb., 9 oz.). She was symmetrically growth restricted — likely secondary to her mother’s chronic hypertension and preeclampsia. She was initially placed on nasal continuous positive airflow pressure, but was then intubated and given surfactant after about 12 hours of life because of worsening oxygenation. The infant responded well to the surfactant and weaned off the ventilator quickly. She was given Vitamin A to prevent chronic lung disease and caffeine to facilitate extubation and treat apnea of prematurity. Ultrasound of her head did not reveal any intraventricular hemorrhage. Enteral feeds were initiated with donated human milk (known to reduce the risk of necrotizing enterocolitis) until the mother’s own milk supply was established.
After two months in the NICU, the baby developed systemic hypertension and an intermittent heart murmur. A technician from Cincinnati Children’s came to the birth hospital to perform an echocardiogram, which revealed a small patent ductus arteriosus with left to right shunting, and normal biventricular function. A renal ultrasound revealed multiple small kidney stones. Cincinnati Children’s nephrology service recommended amlodipine as well as chlorothiazide, which successfully controlled the hypertension. A repeat head ultrasound at discharge revealed no evidence of periventricular leukomalacia, and an ophthalmologic exam revealed mild bilateral retinopathy of prematurity.
Clinical Outcome and Follow Up
After discharge, the infant was brought to the High-Risk Infant Follow-Up Clinic at the birth hospital, and was also seen by specialists at Cincinnati Children’s, including pediatric ophthalmologists and nephrologists. She developed signs of gastroesophageal reflux and was started on Prevacid, with some improvement in symptoms. She had worsening of her retinopathy of prematurity, to stage 3+, but did not require surgical intervention. Her hypertension gradually improved, and she was taken off of the amlodipine, but remains on the chlorothiazide. She will have a full development assessment at six months adjusted age.
Discussion and Lessons Learned
This case demonstrates how a well-organized regional model of care can coordinate the complex medical needs of a fragile preterm infant and optimize the infant’s outcome. Identifying mothers at risk of delivering premature infants and transferring them to Level III centers prior to delivery is crucial to securing the best outcomes for their babies.
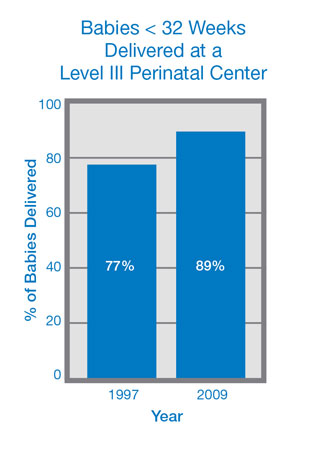
It has been shown in our area (Pediatrics 2004; 113(1); 35-41) and elsewhere in the country that infants <1,500 grams have decreased morbidity and mortality when they are born at a Level III center. Clearly, a transfer while still in utero is safest for these high-risk infants. Following educational outreach in our region regarding this issue, our data has shown an increase in the percentage of infants being appropriately delivered at a Level III center.
A perinatal service with the experience and expertise of caring for a large number of very preterm babies offers mother and infant the best care possible. Evidence-based practices, such as surfactant administration and the use of antenatal steroids, Vitamin A and human milk, can reduce the known morbidities of preterm birth.
The close collaboration of the birth hospital’s Level III nursery with the wide range of subspecialists at Cincinnati Children’s allows the highest level of care without the disruption and risk of transport after birth. This model also allows infants and their mothers to receive all of their care in one nursery (in one bed space, in most cases), leading to strong bonds between the family and the staff and promoting family-centered care.
This case study was written in collaboration with Amy Nathan, MD, Division of Neonatology, Perinatal Institute and medical director, TriHealth Nurseries.