Hope in the Darkest Places
High Stakes Drive Our Unmatched Intensive Care
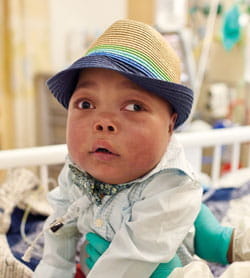
Muhamed curls into his mom’s arms, a small, straw fedora atop his head. It matches his pale green button-down shirt and flowered bow-tie perfectly.
“We like to keep him fashionable,” Hana says, hugging him close. “Every day with him is a miracle.”
That’s because he entered the world sooner than expected. Much sooner.
“Muhamed was born when I was just 26 weeks pregnant,” Hana explains. “He was so small. He had underdeveloped lungs, an immature nervous system— and everything else that goes along with prematurity.”
For the first six months of his life, Muhamed was in the neonatal intensive care unit at his birth hospital in Michigan. “His lungs weren’t able to work on their own, so he needed a ventilator to breathe,” Hana remembers. “That meant he had to have a breathing tube placed in his throat. He also had a feeding tube to get the nutrients he needed.”
After six months, Muhamed needed more specialized care, and was sent to a nearby pediatric hospital. There his condition continued to worsen.
“His doctors thought he might need a lung transplant,” Hana says, her voice softening. “I researched where he could go and found out Cincinnati Children’s was the best place for him.”
In May 2016, nearly a year after his birth, Muhamed was tucked into a transport bed and airlifted to the pediatric intensive care unit (PICU) at Cincinnati Children’s.
Caring for the Most Fragile Patients
Erika Stalets, MD, thrives when she’s busy. That’s why being the medical director of our PICU suits her.
“Children come here for many different reasons, ranging from a severe injury to chronic care needs,” Dr. Stalets says. “But it’s not just medical care we provide — every day we have parents who are afraid that their child won’t come home. We give them the support and reassurances they need in their darkest hours.”
Those high stakes drive our unmatched care. As one of the busiest and most highly regarded pediatric hospitals in the nation, we see some of the most medically complex patients. And the expertise and innovation found here can mean the difference between life and death.
Because of our world-class reputation for care, the demand for our services continues to grow. Our 20-year-old PICU needs to be updated to accommodate these increasing needs — including bigger care teams and new technologies.
“We’re always looking for ways to make the best care of today better for the future,” says Dr. Stalets. “That’s why the Critical Care Building will include three new, state-of-the-art intensive care units — pediatric, newborn and cardiac. These new areas will allow us to better meet our current needs and prepare for growth and advances in care in the future.”
Hope Far from Home
Hana was nervous about being in a new city in yet another hospital, far from family, while her tiny son underwent a lung transplant. How would his fragile body cope with major surgery? How would she?
“I realized quickly that the team at Cincinnati Children’s was amazing,” Hana says. “Before anything else, they wanted Muhamed to get stronger. As he did, they determined that he wouldn’t need a lung transplant anytime soon. For the first time, I felt hope in what had seemed a hopeless situation.”
Through triumphs and setbacks, she stayed by her son’s side. Every minute was precious. Hana remembers, “We spent a long time in the hospital and every single person treated us with kindness and dignity. We were cared for like we were family.”
Centering Families and Staff
Caring for kids and families is what drives Jerry Schwartz, assistant vice president of Patient Services for the PICU.
“Parents have enough to worry about when they have a child in the hospital,” Jerry says. “On average, they spend 21 hours a day in their child’s room. And our current PICU isn’t set up for stays like that.”
Hana agrees. “Muhamed’s care was incredible. But I longed for a better, more private area to sleep and space so I could stay close to my son while eating or working. Because the room was small, I often felt like I was in the way of his providers when they came to check on him.”
It’s not just families that find our current space challenging. Working in the PICU is incredibly rewarding, but it can also be incredibly stressful. The current unit lacks space for staff and care teams to meet, decompress and rest—the new PICU will rectify that.
“When we began talking about the new PICU design, we knew we needed a unit that would accommodate the needs of families and staff,” Jerry says. “We talked with both groups to find out exactly what they wanted, then we used that feedback to ensure the new space meets their needs.”
Bringing Muhamed Home
After eight months in the PICU, Muhamed’s care team began transitioning him to a home ventilator. “I couldn’t believe it,” Hana says, her voice catching. “We might get to take our baby home.”
At 21 months old, Muhamed left the hospital for the first time. This past June, he celebrated his third birthday surrounded by his family. He’s working on taking breaks from his ventilator. He loves music and cuddles — he’s even enrolled in a home-based preschool.
And, although the family has returned to Michigan, his Cincinnati Children’s team still manages his care.
“I’ve slept in hospital beds and lived in new cities far away from my husband and family to get the best care for my son,” Hana says. “We were lucky to find people at Cincinnati Children’s who have Muhamed’s best interests in their hearts. Because of them, our family is together in our home — an outcome that I didn’t think possible before we came here.”