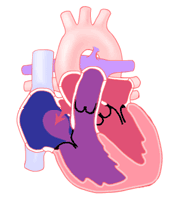
How is ASD Treated?
In some children, an ASD may close on its own without treatment. With a small atrial septal defect, the chance of the ASD closing on its own may be as high as 80% in the first 18 months of life. An ASD still present by 3 years of age will never close on its own.
Open-Heart Surgery
Although an atrial septal defect may be closed by open-heart surgery, this approach is not as common as it once was. If open-heart surgery is necessary, the surgeon may be able to close the hole with stitches. Or it may need to be closed with a patch. Surgery is effective and carries a low risk.
Transcatheter Device Closure
Depending on the size and the area of the septum involved, many atrial septal defects may be closed by a device being put in during a cardiac catheterization. This device is put in through a catheter. It covers the ASD by attaching to the atrial septum. A catheter is a long thin tube, about as wide of a piece of spaghetti. This is directed to the heart through the large blood vessels in the groin.
Atrial Septal Defect Closure Results
Surgical closure of atrial septal defects doesn’t have problems in 99% of cases. After ASD closure in childhood, the heart size returns to normal over four to six months.
After the defect is closed, there should be no problems with activity and no restrictions. Regular follow-up appointments will be made with a cardiologist.
How Are Adults and Adolescents With ASD Managed?
An atrial septal defect can be discovered for the first time in adult life. ASDs come in many sizes. A small ASD may have no significant effect on a person’s health. If ASDs are large enough to cause the right heart chambers to get larger, repair is recommended. Secundum ASDs are the most common form. These can usually be closed without surgery, using a device. The other forms of ASDs require surgical correction. These are typically low-risk procedures. Doctors with congenital surgical experience is important.
Adults who have a closed or repaired ASD need periodic evaluation. Patients who have had device closure of ASDs should have an echocardiogram every five years to look for complications of the device. Patients who had some high blood pressure in their lungs (pulmonary hypertension) before the ASD was closed should continue to see their cardiologist. Adults who have had rhythm problems such as atrial flutter or atrial fibrillation may need regular evaluation.
Learn more about the Adolescent and Adult Congenital Heart Disease Program.