What is Craniosynostosis?
Craniosynostosis, or simply synostosis, is the early growing together (or fusion) of two or more bones of the skull.
Craniosynostosis, or simply synostosis, is the early growing together (or fusion) of two or more bones of the skull.
A newborn's skull is made up of many separate bones that are not yet fused together. The brain grows quickly in the first two years of life. It’s important that the skull bones remain open, so the brain has enough room to grow. Complete fusion of the bones normally occurs late in the teen years. Synostosis interferes with normal growth of the brain and skull.
A suture is the seam between two skull bones. The different skull sutures naturally close throughout a human’s life. Some of these sutures close at a young age. Others may close later in life.
At birth, the open sutures allow a lot of flexibility in the face and skull bones. This flexibility allows the newborn to pass through the birth canal. The bones will settle into a typical shape within one to two weeks after birth.
In many children, the only symptom may be an irregularly shaped head. Some children will experience unusually high pressure on the brain, initially causing headaches. If left untreated, some children may develop learning disabilities or problems with their eyesight. Craniosynostosis causes a change in the normal shape of the head. If a suture − the seam between two skull bones − is fused, it cannot grow. This causes the bones with open sutures to grow more than usual to allow enough room for brain growth.
Early in life the brain avoids damage from this pressure as other bones grow to accommodate the growing brain. Doctors cannot predict which children will develop this pressure problem. With more than one suture fused, the chance of increased pressure is higher.
Children who have multiple suture craniosynostosis, have a higher risk of increased brain pressure. They can experience head pain, damage to the eyes, and developmental delays because of this.
The main symptom of craniosynostosis is an abnormal head shape. An abnormal head shape (plagiocephaly) can happen when forces push on the skull before or after birth. This can happen before birth:
After birth, abnormal head shape is most commonly a result of gravity. This can happen when the baby lies in one position for long periods of time.
Most head shape problems will fix themselves within the first few weeks after birth. The fix is usually rapid brain growth or frequent repositioning of the baby. Repositioning involves moving the baby (usually onto the stomach) to make sure they are not sleeping or lying on one side of the head for too long.
Molding helmets may be used for newborns who are not showing improvement in head shape with repositioning techniques. It is important to recognize positional plagiocephaly (a non-surgical condition) from craniosynostosis, which requires surgery to correct the problem.
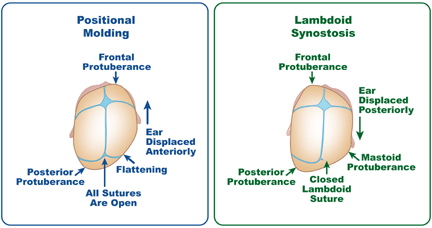
There may be reasons other than synostosis that your child's head is misshapen, so your child's doctor may order X-rays or a CT scan to screen for this condition. The doctor may refer your child to a neurosurgeon or plastic surgeon to obtain an opinion regarding the problem.
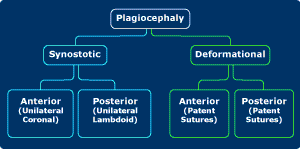
Types of synostosis can include:
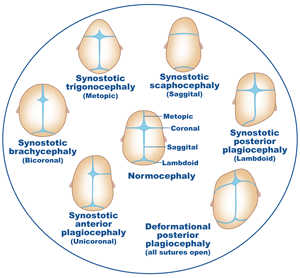
Craniosynostosis can happen on its own without other related abnormalities (non-syndromic). It may stem from an underlying genetic condition (syndromic). The type of craniosynostosis a child has depends on which skull sutures fuse. The child’s head shape looks different based on which sutures fuse.
If one skull suture fuses, the condition is called single-suture synostosis. Examples of single-suture synostosis include:
If two skull sutures fuse, the condition is called double-suture synostosis. Examples of double-suture synostosis include:
In some cases, more than two skull sutures will fuse. These conditions are called complex multisuture synostosis. Examples of complex multisuture synostosis include:
Sometimes craniosynostosis is associated with an underlying genetic condition. These conditions can include:
This is the most common syndrome related to craniosynostosis. It is associated with bilateral coronal craniosynostosis, midfacial abnormalities, forward protrusion of the eyes and airway obstruction. About 30% of patients will have fluid buildup in the brain (hydrocephalus). There generally are no limb abnormalities. Intelligence is often normal. This syndrome occurs in one out of 25,000 births. A mutation that may be responsible for Crouzon's syndrome has been found in the FGFR2 gene. However up to one-third of the cases occur spontaneously.
This syndrome is also related to bilateral coronal craniosynostosis, with a tall and shortened head. Other forms of synostosis may also be seen with this condition. The skull base is frequently fused as well. Hand, elbow, hip and knee abnormalities may also be present. Like Crouzon's syndrome, the face has a classical appearance with protrusion and wide spacing of the eyes, beaked nose and down-slanting eyelids. It occurs in about one in 100,000 births. This is usually an inherited pattern. Developmental delay is common. Intellectual disabilities are seen in 50-85% of cases.
This syndrome is commonly associated with lambdoid and sagittal synostosis. The child may also have limb abnormalities that may include extra digits on the feet. It is also associated with abnormalities of the heart. A genetic location for this syndrome has not yet been identified.
This syndrome is also characterized by craniosynostosis and limb abnormalities. Unicoronal craniosynostosis is common as well as mid-facial deformities, protruding eyes and hearing loss. Fluid buildup in the brain (hydrocephalus) is common. Three types have been described, with types 2 and 3 being the more severe forms.
This is a congenital syndrome that’s often associated with craniosynostosis and limb abnormalities. The genetic location of this syndrome is different than the other syndromes. Characteristic features include coronal synostosis (usually unilateral) with limited growth in the anterior cranial base. Children may also have a low set hairline, eyelid abnormalities, facial asymmetry and mild to moderate developmental delay.
Craniosynostosis is treated by surgery that opens the fused sutures. This creates space for brain growth. A variety of surgeries may be used. The surgeon will discuss the craniosynostosis treatment options available for your child. They will work with you to choose the most appropriate procedure depending on the sutures involved and your child's age when they are diagnosed. A neurosurgeon and a plastic surgeon work together for more complex types of craniosynostosis.
Minimally invasive surgery can be used to treat patients with various types of craniosynostosis. It is reserved only for young infants (younger than 4 months of age).
Patients who have minimally invasive surgery will wear a custom-made helmet for a few months after surgery. The helmet will gently mold the child’s head into a more natural shape as the brain grows.
Endoscopic Craniectomy or Strip Craniectomy: One of the most common types of minimally invasive surgery is an endoscopic craniectomy or strip craniectomy. The surgeon will remove the suture by making small incisions (cuts) on the scalp. A small camera (endoscope) is used alongside the CT imaging to work in exactly the right spot. When used to treat sagittal synostosis, this procedure is called an endoscopic strip sagittal craniectomy.
Cranial Springs: This surgery starts with a strip craniectomy, where the surgeon will remove the fused suture. After that, the surgeon places stainless steel springs in the newly opened suture. This gives the brain room to grow. The surgeon will remove the springs a few months later. This procedure is typically used to treat sagittal synostosis.
Cranial Vault Reconstruction (CVR): The surgeon will remove pieces of the skull near the fused suture and re-shape it to allow room for the brain to grow. A CVR may be done on the entire skull or in individual sections. It is also called cranial vault reconstruction, cranial vault remodeling or cranial reconstruction.
Cranioplasty: A cranioplasty repairs skull anomalies or holes. A surgeon may repair the skull with the child’s original bone (autologous cranioplasty). They may use artificial bone (skull allograft implant) as well.
Distraction (Cranial Vault Distraction or Cranial Distraction): This surgery is used to expand part of the skull, usually the back of the skull (posterior vault distraction or PVR). During the operation, the surgeon will remove a piece of skull. They will put in a medical device that’s secured by screws. The device allows the skull to increase in size. Once enough bone grows back, the surgeon will take out the screws and device.
Frontal-Orbital Advancement (FOA): An FOA removes and reshapes the skull bone around the forehead. It is often used to treat older infants who have a severe metopic synostosis or coronal synostosis.
Before surgery, your child will be scheduled for an appointment with the Craniosynostosis and Cranial Reconstruction Center. This will include neurosurgery and plastic surgery. To help us prepare for a successful surgery, please share your child's full medical history, including any:
Let us know of any unexplained problems with surgery. Watery eyes, sneezing or wheezing while playing with balloons may be due to a latex allergy. Anyone who has had multiple surgical procedures might have this allergy.
If your child needs a helmet after surgery, we will schedule a helmet fitting appointment at the Hanger Clinic. They specialize in creating orthotics and prosthetics. This appointment will happen a week or two before your child’s surgery. We’ll notify you once your child’s helmet is ready. You can pick it up right before or after your child’s surgery.
On the day of the procedure, a doctor called an anesthesiologist will talk to you about methods of pain control that are appropriate to your child's size and age.
The anesthesiologist will get a thorough history of your child's past anesthetics. They will also need to know any family reactions to general anesthesia. On the day of the surgery, please be prepared with this information. It is very important in preventing possible reactions to anesthetics that may be used during the surgery.
Before coming to the hospital, please read the pre-operation checklist below. If your child is old enough to understand, please explain what will happen before, during and after surgery using familiar terms.
If your child takes daily medication for the heart, asthma or seizures, they need to take the medication the morning of surgery. Your child should take medicine with a small sip of clear liquid. Do not give antibiotics the morning of the surgery as they can cause nausea and vomiting.
If you have questions about your child's medication, please call the neurosurgery office at 513-636-4726.
Depending on the type of surgery, your child may go to our pediatric intensive care unit (PICU) right after surgery. Your child's head will be fully wrapped with a turban dressing. Their head will be elevated. Sticky pads on your child's chest give readings to monitor the heart. A red light on your child's finger or toe tells us if the blood is getting enough oxygen. Your child will get needed fluids and medications through their IV. A blood sample will be taken to make sure your child is recovering as well as expected. This will happen about every six hours for a few days.
Your child will be sleepy the first day. They will be able to take a bottle the evening of the surgery. Two days after surgery the head dressing will be removed.
When their blood counts are stable, your child will move from the PICU into a regular room. At this point, you'll be able to hold your child. Their head and face will be swollen. The worst swelling occurs two to three days after surgery. Often their eyes swell shut. This may frighten your child. Parents' voices and familiar music and sounds help comfort your child.
You can take your child home on the fourth or fifth day after surgery if they had cranial vault reconstruction. Most children undergoing minimally invasive craniosynostosis surgery leave the hospital in one to two days after surgery. Head and face swelling will be improved. The swelling around the eyes will come and go for two to three more weeks.
If your child sleeps face down, they will awaken with the eyes swollen shut. After one or two hours, this swelling will go away. To decrease swelling, we recommend that you put your child to sleep on their back for several weeks after surgery. If they roll over, reposition the child onto their back. Keep their head up.
Once home, your child may have the days and nights confused. To lessen the effects of this adjustment, provide periods of play during the day in a bright room.
If your child needs to wear a helmet after minimally invasive surgery, they can start wearing the helmet approximately 72 hours after the procedure. Your child’s doctor and helmet specialist will give specific instructions of when to start the helmet therapy. They will tell you how long your child should wear the helmet each day.
Follow-up appointments are typically two weeks after the surgery. This appointment will either be with an advance practice provider or your child’s surgeon. Three months after surgery your child will have a follow-up appointment with the surgical team.
These appointments should be scheduled before you take your child home from Cincinnati Children's.
If your child has a helmet, follow up will be determined by the helmet specialist. Most children will go to their first helmet follow-up appointment seven to ten days after surgery.
Call the neurosurgery care team at 513-636-4726 if you are concerned with your child's progress after surgery.
Please call if your child has:
Our office hours are 8 a.m. to 4:30 p.m. Monday-Friday. On evenings and weekends, please call the main hospital line at 513-636-4200 and ask to have neurosurgery on-call doctor paged.

Cincinnati Children’s Craniosynostosis and Cranial Reconstruction Center has more than 30 years of experience treating children with craniosynostosis, skull bone abnormalities, and skull lesions. Led by expert neurosurgeons and plastic surgeons, our team works together to provide advanced surgical options and the best possible outcomes for your child.
Last Updated 08/2021
Learn more about our editorial policy.