What Is a Nasogastric Tube Feeding Using a Feeding Pump?
How Do I Know the NG Tube Is in the Right Place?
- Wash your hands with soap and water.
- Check that the NG tube is in the right place:
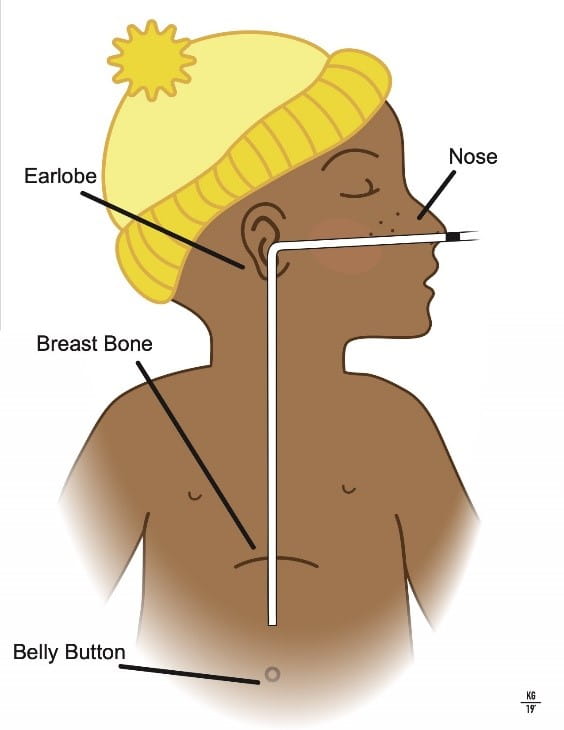
- Measure the external length of the tube and check that this has not changed.
- External length = measurement of feeding tube from nostril to base of the hub OR check the mark that was drawn on the NG tube when the tube was placed, making sure it is right next to the nostril.
- Connect a small enteral syringe to the end of the NG tube and pull back to get stomach contents.
- Do not return the stomach contents back in the tube.
- Flush the NG tube with 3-5 mL of water.
- If you are unable to remove the stomach contents, remove the syringe, close the cover over the end of the tube, and place your child on their left side. After 10 minutes, repeat the attempt to pull back stomach contents into a syringe.
- Do not return the stomach contents back in the tube.
- Flush the NG tube with 3-5 mL of water.
- If you are unable to remove stomach contents, remove the NG tube and reinsert the tube (if you have been taught how to do so).
AND
How Do I Give a Feeding?
- Wash your hands with soap and water.
- Gather the supplies:
- Feeding pump
- Feeding bag
- IV pole
- Farrell valve system bag (if ordered by your doctor)
- Formula or breastmilk
- Bottle or container to measure formula or breastmilk
- Small syringe, 6-12 mL
- Water
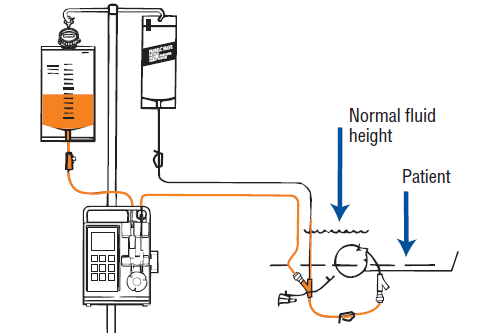
- The Farrell valve system bag (if ordered for decompression).
- Use a new Farrell valve system bag every 24 hours
- Connect the bags at the "Y" junction on the Farrell bag tubing.
- Keep the "Y" of the feeding bag tubing and Farrell valve connection at the stomach level.
- Add the formula or breastmilk to the bag. Add an extra 30 mL of formula when you fill the bag the first time. The extra is for priming the tubing.
- Eight hours for all formula that is in a can or a box and is ready-to-feed.
- Four hours for breast milk, formula that is mixed or prepared, and for immune-suppressed patients.
- Two hours for warmed milk. Warm milk in a feeding pump is not recommended.
- Mixed formula may be refrigerated for up to 24 hours.
- Throw away any formula left in the feeding bag before you add new formula. Do not rinse the feeding bag. Use a new feeding bag and Farrell bag every 24 hours.
- Prime, or fill, the tubing of the feeding bag with formula or breastmilk.
- Stop the formula or breastmilk just before it reaches the end of the tubing.
- This prevents formula or breastmilk from getting into the grooves on the end of the feeding tube.
- Put the tubing into the feeding pump.
- Turn the pump on.
- Refer to feeding pump instructions for pump programming.
- Set the rate – how fast the feedings are to go in
- Set the dose − how much formula or breastmilk is to be given
- Check to make sure the NG tube is in the correct place (see above).
- Connect the feeding bag tubing to the NG tube.
- Start the feeding pump.
- When the feeding is finished, turn off the pump. Pinch the feeding tube then remove the feeding bag and flush the NG tube with water to clear the tube.
- Clean and dry the ENFit connector (moat, cap, lid) daily and when soiled
- Use a toothbrush with water to clean the connector (this toothbrush should only be used for cleaning the tube).
How long can the formula or breast milk be in the feeding bag?
What Other Things Do I Need to Remember?
- If your child begins to choke or gag during a feeding, stop the feeding pump.
- Re-check tube placement.
- When your child is no longer choking or gagging, you may restart the feeding after confirming the tube is in the correct place.
- There is a possibility that your child could throw up and the tube could come out of their mouth. Remove the tape and pull the tube from your child’s nose.
- If your child continues to have trouble breathing, call 911.
- If your child's stomach becomes large and round or if they have discomfort, stop feeding and wait 30-45 minutes.
- If the stomach remains large and round or if your child continues with discomfort, call your nurse or doctor.
- To prevent clogging the feeding tube:
- Flush the feeding tube with water before and after giving a feeding or medication as recommended by your provider.
- Give one medicine at a time, and flush with water between each medicine.
- Check with your doctor or pharmacist before giving any new medicine through the feeding tube.
- Approved pills or powders need to be crushed then mixed with water and fully dissolved before putting into the feeding tube.
- If the feeding tube is clogged, use a small enteral syringe with warm water and try to gently flush the feeding tube. You may need to pull back gently and then push the water in. Use a plunging motion to dislodge the clog.
- If you remove the NG tube, pinch the feeding tube so that formula does not drip from the tube and get into your child’s lungs.
- You can re-use the same feeding tube for up to 30 days.
- Always check the feeding tube for any holes or tears before you reuse it.
- Insurance companies usually cover the cost of two NG tubes a month. NG tubes can be reused if pulled out, if they are clean and still in good condition.
- It is important to help your child enjoy feeding time. You can do this by holding your child, offering a pacifier for sucking, letting them sit in a highchair, and including them at the table for family meals.
- Ask your doctor or nurse about therapy to help improve oral skills.
What Do I Do If Formula/Breastmilk Backs Up Into the Farrell Bag?
If formula or breastmilk backs up into the Farrell bag, this means your child’s stomach cannot handle the feedings or there is a problem with the tubing or the feeding tube.
- Close the clamp on the Farrell bag.
- Check your child to make sure their stomach is not swollen or bloated.
- Check the feeding tube for kinks.
- Check to make sure the feeding tube is not clogged:
- Disconnect Farrell valve tubing from the NG tube.
- Flush the NG tube with a small amount of water.
- Drain the formula or breastmilk from the Farrell bag into a cup.
- You need to do this because you cannot control how fast the formula or breastmilk flows.
- Open the clamp on the Farrell valve tubing.
- Measure the amount of formula or breastmilk not given.
- If your child and the feeding tube are OK, raise the Farrell valve bag higher to avoid having formula or breastmilk back up into the Farrell valve bag.
- If the problem persists, call your provider.
Call Your Doctor or Nurse If:
- Your child is uncomfortable or fussy with feeding.
- Your child vomits or has diarrhea.
- Your child’s stomach is swollen or bloated.
- You are unable to replace the NG tube.