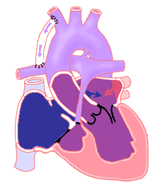
How Are Single Ventricle Anomalies Treated?
What Is Fontan Circulation?
In the normal heart, each ventricle does a separate job. The right ventricle pumps blood to the lungs. The left ventricle pumps blood to the body.
In a single ventricle heart, there is only one ventricle large enough to do the normal job of pumping blood.
Whenever there is only one ventricle large enough to do a normal job of pumping blood, we need to change the circulation to make it the best it can be without overworking it.
In a single ventricle heart, the single ventricle will pump blood to the body. The job of getting blood to the lungs must be done without a pump.
The "Fontan circulation" refers to this configuration where the single ventricle pumps blood returning from the lungs to the body. The blood returning from the body travels to the lungs by blood vessel connections without a pumping chamber. There may be different surgeries needed.
Who is a Good Candidate for Fontan Surgery?
For a heart with a Fontan reconstruction to work well, there are a few features that must be maintained.
The single ventricle must continue to work well. It cannot develop dysfunction (poor squeeze or pumping) because of pumping extra volume or pressure. Your child’s cardiologist will watch the function of their heart with echocardiograms. If the function starts to fall, they may start medicines or order more testing.
The pulmonary arteries must grow well without stenosis (narrowing). They must remain low resistance (or be very relaxed). If the pulmonary arteries are narrow or if the resistance in these vessels is high, blood will not be able to flow into them without a pump. This means the Fontan will not be successful.
Leaky or tight valves may negatively affect the function of the ventricle or the flow of blood to the lungs.
How is Fontan Circulation Achieved?
The type of operation needed in the newborn period depends on the specific type of single ventricle cardiac defect. In some babies, there is not enough blood flow into the lungs. This leads to cyanosis. In these babies, a tube graft is placed from another artery to the pulmonary artery. This is called a systemic to pulmonary artery shunt. It may be called a Blalock-Taussig-Thomas (BTT) shunt. This can sometimes be done non-invasively in the cardiac catheterization lab with a ductal (PDA) stent.
In other babies, the flow of blood into the lungs may be too much. This puts more work on the ventricle. This may lead to very high pressure in the pulmonary arteries. In these babies, a procedure will be done to restrict blood flow to the lungs. This is done by placing a piece of material or a "band" around the pulmonary artery to narrow it. Sometimes this can be done non-invasively in the cardiac catheterization lab with small plugs that can be put into the pulmonary arteries called pulmonary flow restrictors.
Other newborns have more complex heart disease and need more complex operations. This may include the Norwood procedure for patients with hypoplastic left heart syndrome.
Rarely, a baby with a single ventricle defect will have "just right" flow into the lungs. This means that an equal amount of blood flows to the body and the lungs. These babies do not need intervention in the newborn period.
The goal for any baby in the newborn period is to balance the blood flow between the lungs and the body. This leads to stable oxygen levels and good heart function.
The second stage for most children with single ventricle defects is done around 3 to 6 months of age. The operation is called a "bi-directional Glenn" or sometimes a "hemi-Fontan."
During the Glenn operation, the large vessel that drains blood from the head and upper body back to the heart (the superior vena cava) is taken off the heart. It is sewn on to the pulmonary artery. If a prior BTT shunt was present, it is removed. If a pulmonary artery band was previously placed, it may be removed. It can also be left in place.
The Glenn operation has two major advantages in most children. First, since the connection is a direct one between two blood vessels, rather than made of artificial matter, it can grow with the child.
Second, it removes some of the work from the single ventricle. This means the ventricle will no longer have to pump all the blood to the lungs and all the blood to the body. This lessens the risk for early heart failure. The survival rate of this operation is 90% or higher.
After the Glenn surgery, most children will have oxygen saturation levels of 75% to 85%.
The third and final stage in the reconstruction of a single ventricle heart defect is the Fontan completion surgery. This surgery is usually done at 2 to 4 years of age.
During the Fontan surgery, the blood vessels returning blood to the heart from the lower half of the body (inferior vena cava) are connected directly to the pulmonary arteries. Until now, this blood has avoided the lungs. It has been pumped directly to the body leading to oxygen levels lower than normal.
After a Fontan surgery, oxygen levels will be normal (90s). The two most common methods of performing the Fontan completion today are the "lateral tunnel" and the "extra-cardiac" techniques.
In the lateral tunnel method, a tunnel-like patch is put inside the atrium. Blood returning from the inferior vena cava is sent through this tunnel. A connection is made between the end of the tunnel / top of the right atrium and the underside of the pulmonary artery.
In the extra-cardiac method, the inferior vena cava is connected to an artificial tube. It is sewn to the underside of the pulmonary artery. This sends the blue blood flow outside of the heart.
In either method, a hole or "fenestration" may be made between the Fontan circuit and the right atrium. This is there so that if pressures become very high in the Fontan circuit, there is a "pop-off" into the heart. Many fenestrations close on their own many months after surgery. They can also be closed during a cardiac catheterization procedure if needed.
When patients have been well prepared for Fontan completion, the success rates are 90% and higher.