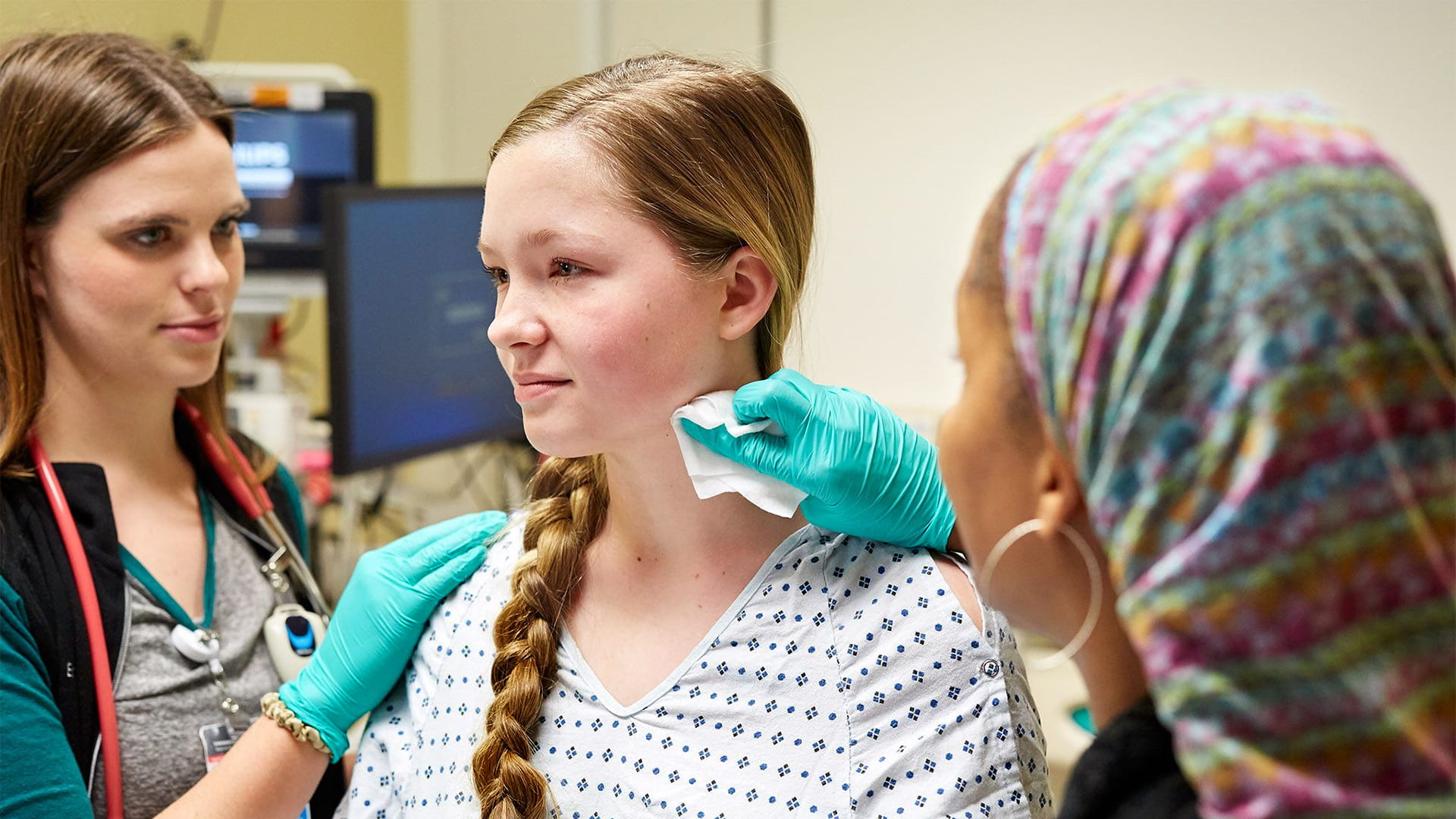
Your Child’s Procedure at a Glance
Cincinnati Children's performs procedures that require anesthesia at our Burnet Campus, Liberty Campus, and Eden Park. Your provider will tell you the location, day and date of your child’s procedure.
Bring these items with you:
- Insurance or medical card
- Your child’s social security number
- Completed pre-procedure physical exam form
- Proof of guardianship (for court-appointed guardians)
- Photo ID for visitors 16 and older, parents, primary caregivers and adult patients
- Completed advance directive paperwork if needed
- List of your child’s medications
- Containers for glasses, contact lenses, hearing aids and dental retainers
- Comfort or distraction items
- Comfortable clothing for after the procedure
- Portable oxygen tank, CPAP or ventilator (if used)
It is best to bring only the child scheduled for the procedure so you can focus on their needs with fewer distractions. If you must bring other children with you, talk to a member of your healthcare team about any guidelines and restrictions that may apply.