Percent of Patients Delayed
Why this measure is important:
- Creating a delay-free system of patient-centered flow that puts the right patient, in the right place, at the right time, with the right team is a foundational building block of safe patient care and it greatly improves the experience of the patients and families that we serve. For these reasons, capacity management and percent of patients delayed is a system wide priority at Cincinnati Children’s.
- Until we are able to optimize and fix the way that patients flow through our system, we will not be able to provide the ideal, safe care and patient experience that we have committed to as an institution.
How we measure:
- This measure reflects the calculated experiences of the patients from the Emergency Department (ED), Pediatric Inpatient Care Unit (PICU), and Post Anesthesia Care Unit (PACU) and is the percentage of ED patients waiting 1 hour or more for admission, patients waiting more than 2 hours for a transfer from the PICU to a regular patient unit and patients waiting 20 minutes or more in the PACU for transfer to a regular patient unit.
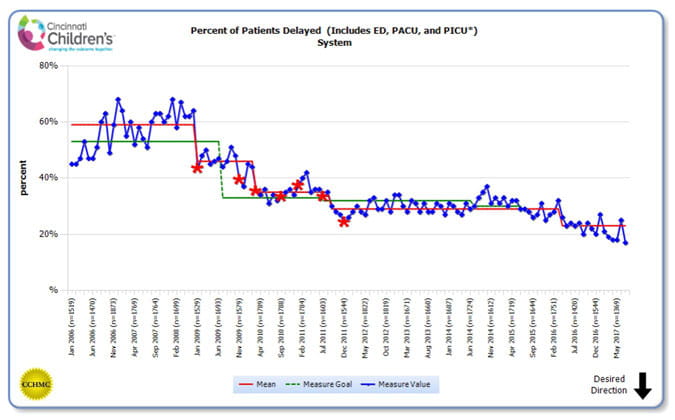
What we are doing to improve:
- Developed an operational planning mechanism that includes daily flow, capacity and staffing planning to meet the needs across our complex and interdependent system and proactively identifies issues that can negatively impact efficient patient flow and safety. Our staff uses predictive and simulation tools and real-time information to make time-sensitive decisions that mitigate operational challenges and effectively allocate resources.
- Implemented a novel approach to discharge efficiency which focuses discharge planning around medical readiness. This system includes standardized discharge goals, which are shared between members of the care team and modifiable based on patient characteristics, allowing for earlier discharge planning. Using high reliability interventions focused on physician and nursing process in the electronic medical records, we have improved timely discharge based on medical criteria for the majority of inpatient services.
- Created a readmissions learning system that engages physicians, nurses and quality improvement experts to systematically identify preventable readmissions, develop targeted interventions and drive improvement across the institution. Using evidence-based solutions, we have improved communication and teamwork across our clinical teams and improved the delivery of information to patients and families that is critical to the post-discharge treatment plan.
View the Operational Definition: Percent of Patients Delayed



