A New Dimension in Care
Surgical Innovations Reduce Risks and Improve Outcomes
Damon, 31, shifts in his hospital bed, his gaze lingering over a picture of himself and his son. A faint smile plays on his lips, as he gently touches the photo where his son, Garrett, is making a silly face.
Clearing his throat, he holds up a different picture, slightly yellowed with age, of a newborn baby. “This is me,” Damon says softly. “Cincinnati Children’s has been following me since I was born.”
That’s when doctors at Cincinnati Children’s discovered Damon had multiple heart defects. He underwent several major surgeries, including a complex procedure when he was 4 years old that allowed his blood flow to bypass a weak part of his heart. At the time, it was his best hope for survival.
And for 27 years, it worked. Damon was able to live a normal life and raise his young son, all while remaining under the expert care of Cincinnati Children’s – first in pediatrics, then in our Adolescent and Adult Congenital Heart Disease Program.
But recently, Damon noticed his heart wasn’t beating normally. His doctors discovered blood clots forming in his heart and lungs. The decades-old repairs were failing, and his life was in danger.
It was time to fix his heart – and, again, Cincinnati Children’s was his best hope.
Surgical Innovation is in Our DNA
Before the 1950s, a baby diagnosed with a heart defect was essentially handed a death sentence. That was, until pediatric cardiologist Samuel Kaplan, MD, cardiac surgeon James Helmsworth, MD, and inventor Leland Clark, PhD, came together at Cincinnati Children’s in 1951. Those pediatric pioneers set out to find a way to make heart surgery safer and a lot more effective.

The heart-lung machine, invented by a team of doctors at Cincinnati Children's, was used to perform the first open heart surgery.
The result was the first heart-lung machine – a discovery that has saved thousands of lives around the world and ignited a firestorm of surgical and heart care innovation.
Today, the Heart Institute at Cincinnati Children’s is building on that legacy, pioneering innovative surgical techniques and technologies – like patient-specific three-dimensional (3D) heart models.
Experts in our advanced imaging group use computed tomography (CT) and magnetic resonance imaging (MRI) scans to make digital 3D models of a patient’s heart. Those files are then sent to the Digital Fabrication Lab at the University of Cincinnati College of Engineering and Applied Sciences to be printed with a special material that produces a nearly exact replica of the patient’s heart.
Holding a Heart in His Hands
It’s an intricate and strangely intimate scene. David Morales, MD, chief of cardiothoracic surgery at Cincinnati Children’s, turns the 3D model of Damon’s heart in his hands slightly, giving the surgical team, clustered around the table, a better angle to see where the first incision will be made. 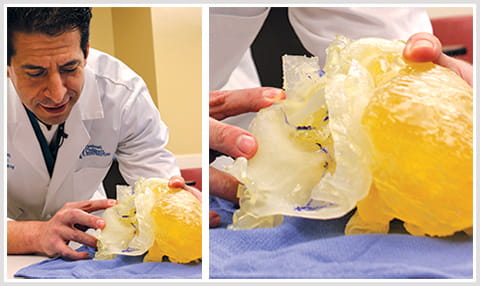
David Morales, MD, looks at a 3D model of Damon's heart to prepare for open heart surgery.
Because the model is so detailed, the team was able to carefully plan and practice the complex surgery and anticipate problems and solutions – all before Damon ever entered the operating room.
“When we walked into the operating room, we all knew exactly what we were going to do,” says Richard J. Czosek, MD, the pediatric electrophysiologist, who helped to stabilize the rhythm of Damon’s heart. “It was remarkable how quickly the surgery went.”
“This is the future,” adds Dr. Morales. “Our imaging capabilities are excellent, but it’s not the same as being able to hold an exact model of the patient’s heart in your hand. This has changed our ability to truly optimize outcomes.”
Moving Medicine Forward
“What impressed me about Cincinnati Children’s is their vision,” says Chuck Mitsui, a generous donor to the Heart Institute. “The team is focused on getting the best minds together, in the best facilities, to move medicine forward to help more kids. And that’s something I want to be a part of.”
 Chuck’s son, Tui, was born with a life threatening heart condition where the four veins that take blood from his lungs to his heart were not attached to the left atrium of the heart correctly. This meant his heart wasn't getting the oxygen it needed. At 24 hours old, Tui was rushed from his birth hospital in Hawaii to Rady Children’s Hospital in San Diego for heart surgery. The surgery was successful, and Tui began to thrive.
Chuck’s son, Tui, was born with a life threatening heart condition where the four veins that take blood from his lungs to his heart were not attached to the left atrium of the heart correctly. This meant his heart wasn't getting the oxygen it needed. At 24 hours old, Tui was rushed from his birth hospital in Hawaii to Rady Children’s Hospital in San Diego for heart surgery. The surgery was successful, and Tui began to thrive.
“Then, at 6 months old, Tui’s doctors discovered some abnormal heart sounds and recommended a second surgery,” Chuck says, his voice growing softer. “But he was growing well and showing no outward symptoms, so we decided to get a second opinion.”
After doing his homework, Chuck learned that Cincinnati Children’s is ranked as one of the best pediatric cardiac care facilities in the nation, so he made the journey from Hawaii to talk with our experts.
“The team in Cincinnati presented us with all of our options. They listened to our concerns, and gave us all that we needed to make a decision that we felt was right for Tui,” Chuck remembers. “It was amazing to be put in that position – where our thoughts and concerns were front and center. We decided to wait to do the surgery – it’s now two years later and he’s doing amazingly well.”
Chuck was so impressed with the compassion for patients and passion for innovation taking place at Cincinnati Children’s that he gave a gift to advance treatments at the Heart Institute. “There’s an energy there, a commitment to advance research and care that’s almost tangible. It’s exciting,” he says. Pictured Above: Mitsuis Family
Providing Hope For a Lifetime
Sixteen days after surgery, Damon headed home, looking forward to his life with his son. “I’ve got a little man to stay strong for. As long as he knows I’m good, that’s all that matters,” he says, his voice catching in his throat.
 That’s exactly what Damon’s medical team kept in mind as they planned his operation. “Planning made a huge difference in Damon’s surgery,” says Gruschen Veldtman, MD, Damon’s cardiologist at Cincinnati Children’s. “What’s really important, though, is that this has added a good number of years to Damon’s life before he may need another procedure.”
That’s exactly what Damon’s medical team kept in mind as they planned his operation. “Planning made a huge difference in Damon’s surgery,” says Gruschen Veldtman, MD, Damon’s cardiologist at Cincinnati Children’s. “What’s really important, though, is that this has added a good number of years to Damon’s life before he may need another procedure.”
The success of Damon’s surgery is the first step on a journey to create the vibrant future our experts see for all of our patients.
So far, Cincinnati Children’s has created 20 patient-specific 3D hearts to plan for complex procedures. With each new model comes the potential for both surgical advancement and better outcomes.
But we can’t do it alone. Support from donors like Chuck is crucial to advancing surgical innovation, like the 3D models, in pediatric care – and not just for the kids at Cincinnati Children’s, but kids everywhere.
“Pediatric cardiology is a small, tightly knit community and any advancement is shared among hospitals,” Chuck says. “By empowering innovation within the Heart Institute at Cincinnati Children’s, I believe I’ll help to improve care for kids like my son around the world – and that’s the real goal. To make a world where kids born with broken hearts will have active, healthy futures no matter where they are.” Pictured Above: Damon and his son Garrett.
We invite you to be a part of these efforts. To learn more, contact Lauren Bosse at 513-803-0639 or lauren.bosse@cchmc.org.
The Breath of Life
When the doctors at Cincinnati Children’s first saw Ghadah, she was 11 months old and only weighed 10 pounds – not much more than many newborns. She was tiny and malnourished, having spent much of her young life in a critical care unit with a breathing tube, on mechanical ventilation.

Ghadah’s family traveled from Saudi Arabia to access our pulmonary medicine program – currently ranked as No. 1 in the country by U.S. News and World Report – when their daughter needed a lung transplant. Photo: The Enquirer/Meg Vogel.
Ghadah suffered from interstitial lung disease. A genetic mutation caused her lungs not to produce enough surfactant, the substance that allows the lungs to easily inflate and deflate and protects them from bacteria and viruses.
The only cure was a lung transplant – and her parents knew Cincinnati Children’s was her best hope. So, they traveled from Saudi Arabia to make sure their daughter received the most advanced care possible.
Three months after arriving at Cincinnati Children’s, Ghadah was finally strong enough for her transplant. With Marc Schecter, MD, and David Morales, MD, medical and surgical director of Cincinnati Children’s Lung Transplant Program, respectively, at her side, she was in the best possible hands. Collectively, they have performed more than 100 pediatric lung transplants.
Ghadah’s transplant was a first for Cincinnati Children’s, but the medical center’s three-year goal is to become a surgical destination center, performing 10 or more lung transplants each year. What’s more, this program also will make it possible for the medical center to perform heart-lung transplants and other multiple organ transplants when needed.
“What makes our program stand out is the multidisciplinary medical team and our ability to perform transplants on infants as small as 11 pounds,” says Dr. Schecter.
Today, Ghadah is a thriving and happy 23-month-old, who smiles at anyone and everyone she sees. Thanks to the expertise and innovation of Cincinnati Children’s, Faleh, her father, will get to see his baby girl grow up.
“Cincinnati Children’s offered more than we ever could have expected,” says Faleh. “Going from a ventilator to full recovery is something that I just can’t describe. I hope to see her at school. I hope to see her working. I hope to see her as a bride.”




