What is Sudden Cardiac Arrest?
Sudden cardiac arrest (SCA) is when the heart suddenly fails to pump blood. If the person does not survive, the term sudden cardiac death (SCD) is used. The person may or may not have a known diagnosis of heart disease.
Sudden cardiac arrest can happen at any age. It is the leading cause of death in teenage athletes in the United States and accounts for approximately 7% of all deaths in the young. Fortunately, SCA and SCD are not common; however, they have a devastating impact on families, care providers and the community.
Causes
Sudden cardiac arrest is caused by a failure in the heart’s electrical system, which keeps the heart pumping normally. Once the heart fails, the rest of the body does not get the blood it needs to function.
Some of the things that may cause sudden cardiac arrest include:
- A sudden blow to the chest
- An allergic reaction or medication interaction
- Breathing trouble such as a severe asthma attack or choking
- Electrocution
- Heart disease or a heart rhythm problem
Many different kinds of heart disease can result in SCA and SCD. Coronary heart disease (CHD) remains the most common cardiac cause of sudden unexplained death in people of all ages. Coronary heart disease is caused by the build-up of plaque in the coronary arteries. These arteries supply blood to the heart. The plaque can reduce or block the flow of this oxygen-rich blood to the heart, causing a heart attack.
Conditions that are more likely to cause SCA/SCD in teens include:
- Hypertrophic cardiomyopathy − Hypertrophic cardiomyopathy is a type of heart muscle disease that causes the heart muscle to thicken (hypertrophy). This thickening typically occurs in the lower-left chamber of the heart, called the left ventricle. This is the most common cause of SCD in young athletes and has been identified in about 30% to 40% of cases.
- Congenital heart disease − Congenital heart disease is a difference in the structure of the heart that is present from birth. Structural heart defects account for approximately 10-15% of SCD cases and include coronary artery anomalies, aortic stenosis and mitral valve prolapse.
- Arrhythmogenic cardiomyopathy − Arrhythmogenic cardiomyopathy is a type of heart muscle disease. This condition causes part of the heart muscle to break down over time, increasing the risk of an abnormal heartbeat (arrhythmia) and sudden death.
- Arrhythmias − An arrhythmia is any variation from the normal rhythm of the heart rate or heartbeat. Two of the more common inherited arrhythmias associated with SCA/SCD include long QT syndrome and catecholaminergic polymorphic ventricular tachycardia.
These diseases are typically undetected prior to the SCA/SCD event. In the case of SCD, an autopsy is essential; however, no identifiable cause is found at autopsy in up to one-third of young people. Lack of knowledge about the cause of SCD poses the greatest challenge in understanding the risk of SCA/SCD for surviving relatives.
Who is at Risk?
Assessing a young person’s risk of SCA/SCD requires consideration of both personal and family history. Children may be referred to a cardiologist for evaluation based on personal risk factors for SCA/SCD such as a history of passing out or seizures that occur with exercise, excitement or startle.
Factors that contribute to the risk of CHD - including tobacco use, high blood pressure, high cholesterol, unhealthy weight, diabetes, non-active lifestyle and excessive alcohol use - are important in evaluating risk for SCA/SCD among individuals of all ages.
Children may also be referred for evaluation based on a family history of sudden death or knowledge of a specific cardiac diagnosis, such as hypertrophic cardiomyopathy or long QT syndrome, in a close relative (parent, sibling).
Signs and Symptoms
Often times, there are no warning signs prior to a SCA/SCD. Many individuals who experience SCA/SCD, however, report experiencing symptoms, such as fainting, before the actual cardiac event. Family history can be an important warning sign, as about 40% of people experiencing a SCA/SCD report a family history of heart disease and about one in four individuals report a family history of SCD before age 50.
Screening
Sports activity has been linked with an increased risk of SCA and SCD in individuals with personal or family risk factors. Recommendations for screening in athletes were published initially in 1996 and have been reviewed and updated. The 12 Element AHA Recommendations for screening include a relative's early death before age 50 due to heart disease, and a known diagnosis of heart disease in a close relative younger than 50 years of age. The degree of relation to the person in the family with heart disease is important. The closer the relation, the greater the potential for risk of SCA and SCD. Athletes with potential increased risk based on the AHA Recommendations should be referred for further evaluation. For non-athletes, routine well-child visits are the standard of care in the United States. However, current recommendations for screening for SCA and SCD are not well defined. It is important to share your family history of heart disease or SCA/SCD with your child’s doctor.
After a SCA/SCD occurs, the evaluation of surviving family members should proceed in a logical and stepwise manner. A detailed family history of the deceased is important, and information must be gathered from available medical records or post-mortem examinations to determine the cause of death. In some cases, the cause of death remains unknown. In this case, a more complete heart evaluation of family members, with echocardiogram, electrocardiogram and lipid screening, may be indicated. In addition to confirming the cause of sudden death in the family, the degree of relation to the deceased individual is important. Further evaluation is most often indicated for first-degree relatives (parents, siblings and children). While families are often anxious and worried after a SCA/SCD, recommending and receiving normal heart testing results may provide false reassurance if the cause of death is not known. If a heritable cause for SCA/SCD is likely, then it may be wise to involve genetic counseling as a first step in risk assessment.
Genetic Testing
Identifying the cause of SCA/SCD is important and necessary in order to provide accurate information to family members. In the case of SCD, ensuring that the medical examiner obtains and stores a sample available for genetic testing is important. One barrier to post-mortem genetic testing has been lack of an available blood sample from the deceased individual.
If the cause of SCD is confirmed, either because of known heart disease before the SCD event or post-mortem diagnosis, genetic testing should be performed based on the specific diagnosis. If a genetic cause is found, family specific testing should be offered to relatives. Clinical genetic testing is available for a number of heart diseases associated with an increased risk for SCA/D. Initiating genetic testing in an unaffected individual is typically not recommended, it is difficult to interpret the results and results are unlikely to be helpful in diagnosis, risk assessment and management.
Post-mortem genetic testing can be helpful in cases of sudden unexplained death. In cases of sudden unexplained death with normal autopsy, post-mortem genetic testing may reveal a cause of death in approximately one in four cases. Long QT syndrome (LQTS) and another inherited arrhythmia, catecholaminergic polymorphic ventricular tachycardia (CPVT), are the most common genetic causes of sudden unexplained death. Both LQTS and CPVT are passed from one parent to a child, so 50% of a person’s children may have inherited a gene mutation. But, they may show normal cardiac test results. Another major function of such testing is reassurance of relatives who did not inherit the disease-causing mutation and avoidance of unnecessary screening and treatment.
Treatment
Quick care during a sudden cardiac arrest will greatly increase the chance of survival. The first step in treatment is to get medical help. Call 911 immediately. CPR (cardiopulmonary resuscitation) and an AED (automated external defibrillator) can increase the chance of survival by 75%.
CPR
CPR provides a flow of blood and oxygen to the brain and vital organs during a sudden cardiac arrest. Classes to learn CPR are available at Cincinnati Children’s (513-636-1096) and in most communities.
AED
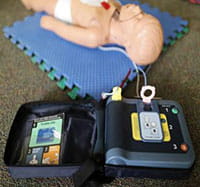 An AED can bring back a normal heartbeat during a sudden cardiac arrest. AEDs can be found in public places such as schools, shopping malls, businesses, airports, hotels and sports venues. AEDs are easy to use and provide audio step-by-step instructions.
An AED can bring back a normal heartbeat during a sudden cardiac arrest. AEDs can be found in public places such as schools, shopping malls, businesses, airports, hotels and sports venues. AEDs are easy to use and provide audio step-by-step instructions.
For individuals known to be at an increased risk of SCA/SCD, medical therapy may be recommended, and in some cases, can provide protection. In some instances, avoiding certain risk factors like participation in competitive athletics may be important. And for those individuals determined to be at high risk for a SCA/SCD, an implantable cardioverter defibrillator (ICD) may be recommended. Most cases of SCA/SCD occur in individuals who were not aware of their increased risk and not under the care of a physician.



