Khurana Hershey Lab
Multidisciplinary Research Approach for Understanding Mechanisms of Asthma Progression
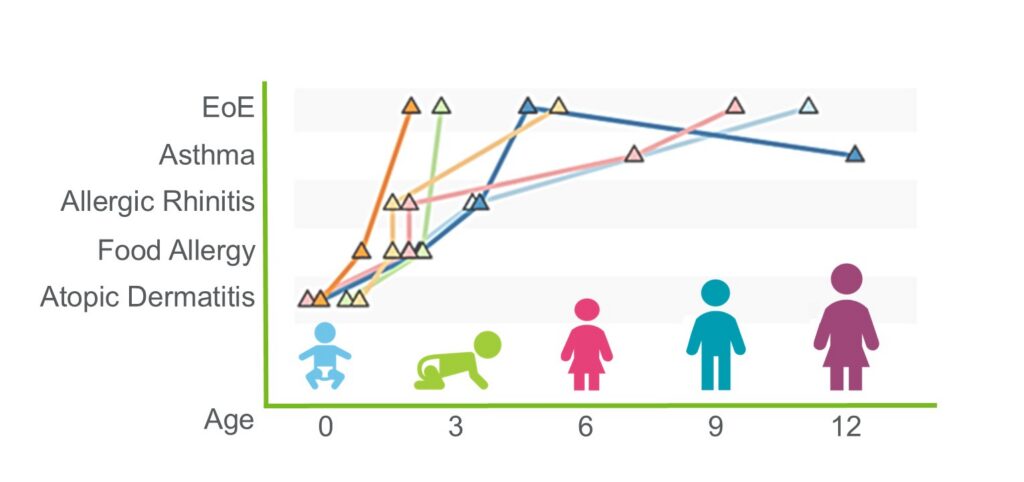
The “atopic march” is a typical progression of allergic diseases that frequently begins during early life. Atopic dermatitis (AD) is largely considered to be the first step in the atopic march, whereby AD typically predates the development of other allergic disorders. AD is a chronic, inflammatory skin disorder that affects up to 20% of children worldwide. Importantly, it has been estimated that one-third to half of patients with AD will develop asthma. Yet, the mechanisms that promote disease progression from AD to asthma remain unclear. Thus, to improve diagnoses and identify novel strategies for prevention and treatment for children with asthma we study the progression of AD to asthma in children. As such, we have built the first mechanistic longitudinal cohort study of pediatric AD, the Mechanisms of Progression of Atopic Dermatitis to Asthma in Children (MPAACH). Using samples from the MPAACH cohort, we integrate clinical, epidemiologic, basic, translational, and multi-omic bioinformatic approaches to accomplish our research goals.
An emerging area of interest for us is understanding how innate and adaptive immune mechanisms are linked to progression through the atopic march. Further, as many biological systems are involved in allergic diseases, we are not only interested in how the immune system impacts disease risk, but also how alterations in epithelial genes, and patient microbiomes play a role. Our current work is exploring more multi-omic and bioinformatic approaches to uncover the cellular and molecular processes that contribute to dysregulation and dysbiosis which ultimately drive allergic disease progression.
Our research is focused on addressing clinically relevant questions and seamlessly utilizing epidemiologic, human, animal, and bioinformatic approaches to discern mechanisms that drive progression of the atopic march. Using these approaches, we can identify novel targets for prevention of allergic disease development and therapeutic intervention for all children, including those most impacted by health disparities. Our work has improved asthma diagnosis, identified new strategies and drug targets, and helped inform new environmental policies to improve child health.
Meet the PI

Gurjit "Neeru" Khurana Hershey, MD, PhD
Science Blog
EoE: The Fifth Member of the Atopic March
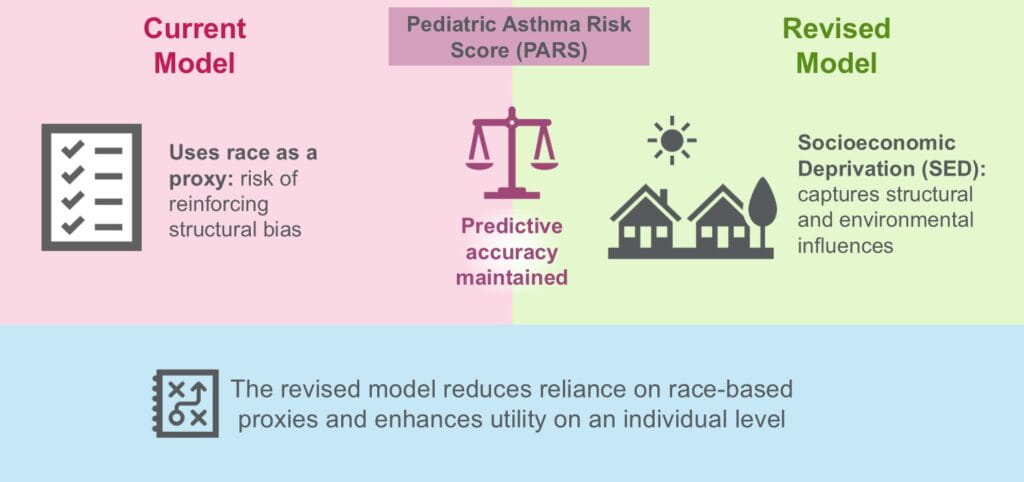
A ‘Must Read’—An Update on Asthma Prediction
Childhood Wheeze Patterns Linked to Distinct Asthma Subtypes Later in Life
Gurjit Khurana Hershey, MD, PhD7/9/2025