What Are Botulinum Toxin Injections?
Botulinum toxin injections are shots given into the muscle (intramuscular injections) to reduce spasticity and involuntary movements in certain muscle groups. These are done in children and adults.
Botulinum Toxin Injection Session
The injection session for botulinum toxin is brief and focused on giving the shots. No other information or exam is needed at this time. In the Division of Pediatric Rehabilitation at Cincinnati Children's the normal process for the session is:
- Caregivers apply a special numbing cream (EMLA local anesthetic) to the sites about one to two hours before the session time. This makes putting the needle into the skin painless. Teaching on this is done at the prior visit.
- The numbing cream is wiped away at the session. The patient is positioned on an exam table for the injection. The sites are cleaned with alcohol. A special spray (topical coolant) is also used to make sure the site is fully numb.
- The smallest diameter needle (27-gauge needle) is used for injecting the medicine. The botulinum toxin needs to be spread out in the muscle, so four or five sites for a large muscle group are often used.
- The total time until it is done is less than one to two minutes.
- The patient will be watched for a short time after the session. Then they can go home and return to normal activities.
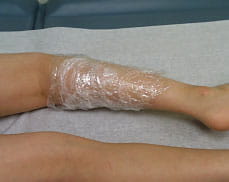
EMLA cream applied to calf muscle with plastic wrap covering.
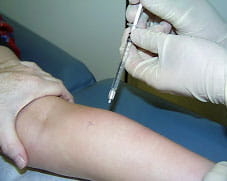
Botulinum toxin being injected into a calf muscle.
Medicine for Relaxation / Topical Anesthetic
Sedation is not often used because the injection time is so short. A local numbing cream (anesthetic) is used instead. Young children often behave as if no numbing cream was used. This may be due to not fully understanding what is being done and having a fear of "shots." In these cases, gentle holding (restraint) is done to keep the area of the shot still. Two staff members sometimes give the injections at the same time to decrease the time of the session.
The EMLA cream does a great job numbing the skin, but the patient may feel pressure and a dull feeling of the needle in the muscle. We know this because we have tried it on ourselves (without the Botox). The EMLA cream will numb the skin to the point of not feeling the shot as the needle goes through the skin.
Medicine to help the patient relax may be given in cases where the patient has not handled shots well in the past. If the patient has another procedure coming up, these shots can often be done at this time. Let the Rehabilitation Medicine office (513-636-7480) know if a procedure or surgery will be done in the future or if sedation is being discussed for injections in the clinic setting.
Possible Side Effects
Injections of botulinum toxin are most often well tolerated without significant side effects. There can be small dots of blood at the sites and some minor bruising. The muscles injected can be weakened more than normal. This is considered a side effect. Since the effects of the botulinum toxin injections are temporary, this will improve over time.
There are no limits on therapy or activity after the session. For patients that don’t normally use a device to help them walk, at first it may seem like their walking has gotten worse. They need some time to get used to the feeling of the sudden change in the way their muscle contracts when they walk. This most often improves quickly over one to two weeks. Some very young children may have discomfort in their heel cord from rapid stretching. The child may limp or refuse to put weight on it. Again, this most often resolves quickly in the first week.
Severe side effects are very rare but can happen if the botulinum toxin unexpectedly spreads throughout the body from the site of the shots. This can cause muscle weakness, hoarseness or trouble talking, trouble saying words clearly, loss of bladder control, trouble breathing, trouble swallowing, double vision, blurred vision and drooping eyelids. The breathing and swallowing problems can be life-threatening. If this happens, seek medical attention right away.
If there are any concerns after the botulinum toxin injections, call the Division of Rehabilitation Medicine (513-636-7480). A follow-up visit with a doctor from Rehabilitation Medicine will be scheduled.
Points of Interest
Interesting facts about botulinum toxin injections:
- First used in eye muscles in the early 1980s
- No long-term problems from injection have been noted to this point
- FDA approved for health problems with eye muscles. Safe and effective non-label use for other muscle groups such as those in the arms and legs
- Can be done in clinic setting
- Repeat injections can be done after three months
- There is no limit to number of repeat injections
- Do not interact with medicine the patient may be taking. No studies have been done on effects on a fetus during pregnancy
- Can be combined with surgical approaches
Frequently Asked Questions
What is muscle spasticity?
Muscle spasticity can be a significant functional problem in children with any injury or disease of the brain or spinal cord (central nervous system, or CNS). With injury to the CNS, the nerves to muscles outside the CNS (peripheral nervous system, or PNS) are no longer under voluntary control by the brain.
When this happens, the nerves of the PNS begin to activate muscles on their own without the control that is usually provided by the brain. As a result, the muscle can begin contracting without relaxation, which causes spasticity.
The spasticity is shown by an increase in muscle stretch reflexes (for example, knee jerk with tapping of the tendon) and clonus (rhythmic, repetitive movement of a joint when its muscle is stretched and held all of a sudden).
When moving a spastic limb through its range of motion, one feels a resistance to movement that increases with the speed at which one moves the limb. This is the definition of spasticity, but other terms such as increased muscle tone, hypertonicity, spastic dystonia, or flexor / extensor spasms are used to describe this resistance. In clinic the term "muscle spasticity" will be used to reduce confusion of terms.
Why treat muscle spasticity?
If spasticity is untreated it can progress to a permanent, contracted state with joint deformity. This is even more of a concern in joints where a muscle group that moves the joint in one direction is much more powerful than the muscle that moves the joint in the opposite direction (muscle imbalance).
This imbalance can affect a joint in varied ways such as at the ankle with foot position (always points toes or up on toes when walking) or at the wrist with hand position (hand in flexion with problems grasping). After a contracture occurs (not able to bring the joint through its full range of motion, even with forceful / prolonged stretching) it can be hard to re-establish full range of motion at that joint without surgery.
Aggressive, early treatment of spasticity is needed to prevent contracture and allow a child to reach their best potential functional activity.
How are contractures prevented?
Prevention of contractures begins with finding out what is limiting a child from either actively (moving oneself) or passively (being moved by someone else) moving the joints through a full range of motion. In some cases, this can be due to destruction or abnormality of the bones around a joint. It can also be due to problems with the ligaments and tissue around that joint.
With abnormal joint movement and inactivity, muscles can shorten and contract. In the case of muscle spasticity, the joint and soft tissue can be normal, but with constant contraction of a muscle because of spasticity the muscle can shorten. When it can no longer stretch to allow full range of motion, a contracture can happen. Agents that lessen the spasticity of the involved muscles best prevent this type of contracture.
What is the benefit of treating muscle spasticity?
Each patient has their own goals for treatment of muscle spasticity made in our clinic. These goals can include decreasing pain from muscle spasms. This can be done by reducing both how often and how intense the spasms are. It can also be done by increasing the range of motion of joints to allow improved function. Improvement of range of motion can help to:
- Improve hygiene: easier toileting and bathing
- Improve fitting of orthotics (braces and splints)
- Improve functional activity: seat position, standing, walking, upper extremity use
- Possibly delay surgery to lengthen tendon to a time when the outcome would be better
How can the spasticity be treated?
To reach these goals, an in-depth evaluation needs to be done for that child to decide how to best manage the spasticity. Therapists are often the first to do an in-depth evaluation of a child with impairments due to spasticity.
Stretching programs with a therapist and encouraging good alignment and positioning for functional activities are most often the first things done to address muscle spasticity. If range of motion continues to be a problem, further evaluation by a doctor who has experience with muscle spasticity could be helpful.
After this evaluation, a doctor may prescribe oral medicine that can reduce spasticity in muscles. These medicines are most helpful in children who have widespread muscle spasticity. These oral medicines spread throughout the body and affect all muscles (skeletal muscles, not muscles as in heart or blood vessels) to some degree.
In many children, there are a few muscle groups that can have very active spasticity. A more focal approach to these muscles would be better than a widespread approach. In this case a doctor may advise a nerve block to interrupt the signal to the muscle that is spastic. Once the signal that is carried to the muscle by the nerve is interrupted, the spasticity will decrease.
There are several types of nerve blocks that can be used to decrease spasticity. This includes phenol, ethanol and botulinum toxin. Of these, botulinum toxin is the best for spasticity relief with ease of use and fewer problems.
What is botulinum toxin and where does it come from?
The botulinum toxin is the same toxin that can develop from bacteria in improperly canned foods. But the botulinum toxin used for injection is purified from this bacterium, clostridium botulinum. It is freeze-dried for future use.
The toxin was first used for medicine in the late 1970s. It was used for injection into eye muscles but was first purified in the 1940s. There are eight types of botulinum toxin that have been isolated from the clostridium botulinum bacteria. Type A is the most potent.
Botulinum toxin type A (BTA) is sold under several brand names. This includes Botox, Dysport and Xeomin. There is also botulinum toxin type B (BTB). This is sold under the brand name Myobloc. The Division of Rehabilitation Medicine at Cincinnati Children's routinely uses the Botox brand of BTA.
When is botulinum toxin used?
After an exam by a therapist and doctor, botulinum toxin for focal relief of muscle spasticity can be advised as the best way to address a child's functional problems. The problem muscle groups are identified, and goals for that child are discussed. Then the injection of botulinum toxin can be done if there are no permanent contractures of the muscle groups.
It is vital that the doctor and therapist discuss when these injections are done. Increase in therapy frequency and change in bracing or splinting may be needed after the procedure.
Therapy after botulinum toxin injections is always done to take full advantage of the reduced spasticity.
How is the botulinum toxin given?
The procedure of injecting botulinum toxin is simple. It does not differ much from injections of other medicines. It is important to decide the potential outcome, based on muscle groups injected, before injections are done.
Other decisions needed include: how much botulinum toxin to use, how many sites to inject, and how concentrated the botulinum toxin should be. An appointment for injection of botulinum toxin is made after this is clarified.
A concern of both parents and children is whether these injections will be painful. There is no pain linked to the action of the toxin itself, only with the needle injections. To lessen this problem, the skin where the injections will be done is coated with EMLA cream before the procedure. A topical coolant spray is also used right before the needle is put in. This numbs the skin. The child may still feel pressure from the needle and a dull feeling in the muscle. The fact that a child is having a procedure done and is being held in place can upset a child more than the needle going in, even more so for preschool-aged children.
Children do very well after having this procedure in our clinic and are not upset when they leave. We rarely use sedation. We use distraction and a quick injection method instead. In rare cases, localization of a muscle may be needed using an electromyograph (EMG) machine or electric stimulator. If this is needed we will discuss this before scheduling the injections.
Are there any problems from these injections and are they lasting?
There are no limits in activity after the botulinum toxin injections. Children can return to their normal activity and therapy. The toxin will start to work within a few hours. Changes in spasticity may last for up to one to two weeks.
A follow-up visit is most often scheduled at around three months after injection. The team will determine if it was helpful and if the effect is wearing off. The effect on muscle spasticity by botulinum toxin is temporary and can last for up to three to five months. This also varies with the amount of toxin injected, the size of the muscle, the degree of spasticity in the muscle, and treatment such as therapy and bracing.
Many times, effects on spasticity are longer lasting. It is not clear if this is due to breaking down patterned movements (many muscles contracting together rather than singly) or from allowing weak muscles to get stronger over time (that were overpowered before by more spastic muscles pulling against them). It is vital to have close follow-up after the injections to figure out the best course of treatment.
Re-injection of the same muscle groups can be done. There are no restrictions to re-injections as long as they are at least three months apart. Keeping injections this far apart lessens the risk of the immune system forming antibodies. These antibodies are not harmful to the child but can make future injections ineffective.
There have been no reports of significant long-term problems in patients that have injections to eye muscles. This has been done since around 1980.
More Information
Botulinum toxin injections are one approach to the treatment of muscle spasticity. These injections can be given with ease and have minimal side effects. They can also be used in very focal spasticity problems that involve a few muscle groups. This treatment may not be right for some patients, such as patients with severe, widespread muscle spasticity, and patients with permanent muscle contractures that have become rigid.
Botulinum toxin injections may be used with other muscle spasticity treatments to get the best total reduction in spasticity to allow functional gains in children.
In some cases, weekly casts of a joint over several weeks (serial casting) will be advised after doing the injections. This is most often done at the ankle and will be discussed before having the injections. We will coordinate the start of casting and the botulinum toxin injections.
You can get more information from the Rehabilitation Medicine office at Cincinnati Children's. Call 513-636-7480 (toll-free 800-344-2462, ext. 7480), option 3. Appointments can be made with any doctor in the Rehabilitation Medicine Division by calling 513-636-7480, option 1.
Scheduling a Treatment
Once the decision is made to do botulinum toxin injections, a clinic visit needs to be scheduled with the Division of Rehabilitation Medicine. Call the office as soon as you can if you decided at the visit to call in later with your final decision.
It takes some time to complete pre-authorization. The sooner we know of your decision, the sooner an injection time can be scheduled. Details of the procedure are worked out during the prior clinic visit and pre-authorization done (if needed) before scheduling the injection session.



