Impaired Barrier Function
The epithelial barrier provides a key checkpoint to prevent penetration of pathogens and antigens, including potential food allergens, from activating the adaptive immune system. We are investigating acquired and genetic etiologies of impaired barrier function and the mechanism by which it contributes to allergic inflammation.
Esophageal Allergy as Protease-mediated Disease
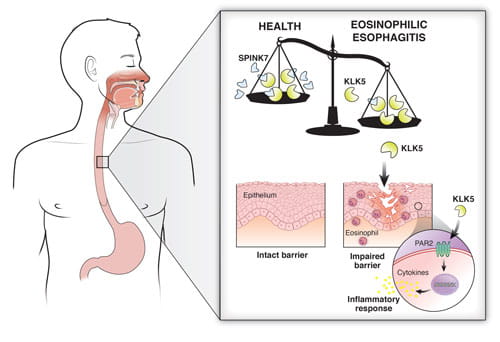
An imbalance of specific proteins, proteases and protease inhibitors, in cells lining the esophagus may cause inflammation and tissue damage in people with eosinophilic esophagitis (EoE). In people with active EoE, biopsies of esophageal tissues show a near-complete lack of the protease inhibitor SPINK7, which normally damps down inflammation and helps preserve tissue structure. In this study, researchers of the Azouz Lab and Rothenberg CURED Lab found a missing link that further explains how the process works. SPINK7 normally binds with the protease KLK5, keeping it in check. Without enough SPINK7, KLK5 is free to degrade tissues and start signals leading to inflammation. These findings highlight esophageal allergy as a protease-mediated disease, suggesting that disarming of proteases by delivering protease inhibitors has the potential to be therapeutic in allergic disease.

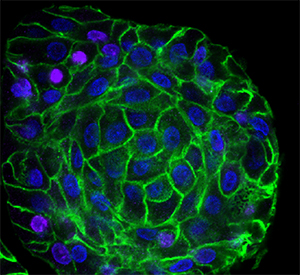
Hematoxylin and eosin-stained sections of control or kallikrein 5 (KLK5)-overexpressing epithelial cells (EPC2) after air-liquid interface differentiation (Day 14) showed dilated intercellular spaces (arrows). Kallikrein 5 is a protease that may play a pathogenic role in eosinophilic esophagitis (EoE). Learn more.
Current Projects
- Role of impaired barrier function in development of allergic inflammation
- Mechanism of impaired barrier function, with focus on acquired and inborn errors in desmosomes
- Role of protease inhibitors such as SPINK7 and related proteases such as kallkikreins
- Interaction of calpain 14 (CAPN14) and barrier formation with focus on DSG1 and filaggrin (FLG)

Proteases and Protease Inhibitors in the Esophagus
A schematic illustration of the potential role of the balance between proteases and protease inhibitors in the esophagus. Downregulation of protease inhibitors unleashes uncontrolled proteolytic activity. Proteolytic activation can lead to innate immune responses, which in turn promote type 2 immunity.
In addition, increased proteolytic activity can result in degradation of junctional proteins and an impaired epithelial barrier.
As a result, antigen-presenting cells show increased access to external antigens and promote type 2 immunity. Learn more.